PATRICK'S
CONCERNS
To avoid spam, my eemale addresse is in .gif image, so type this
manually into your
emayel brow zer.

Latest update on health concerns 28 February 2021.
Hi folks,
The Psa graph below shows that Psa is increasing at a rate that
looks uncontrollable.
Lu177 did
whatever it could do for me in 6 doses, and many mets were
killed and healed
up but a few kept growing, and a few new bone mets appeared
which did not make enough
PsMa expression to justify having any more Lu177. That was the
doc's conclusion last November.
My recent scans have shown I
only have Pca in my bones, so I thought if I could get Ra223
it could be a cancer killer, and prevent pain as my skeleton
began to have micro-fractures or
large fractures due to cancer weakening my bones and causing the
outer layers of strong bone
material to become thin or die.
My oncologist tried to get local Ra223 ( Xofigo ) for me in
in Canberra but the doctor who
was providing it has stopped doing it probably because of a lack
of local demand, and it
was more expensive than Lu177 and not covered by PBS or insurance,
and it can only
be used for palliative care for bone cancer, or perhaps to extend
life a bit longer in patients
with only bone cancer.
So after 2 weeks delay trying to get Ra223 locally, I was able to
arrange getting Ra223
from Theranostics Australia administered at Waratah Private
Hospital at Hurstville in Sydney,
and I had my first infusion on Friday 26 February.
The doctor there who supervised my treatment is well aware of the
risks, well informed,
and explained what was going on and what was likely to happen very
well and administered
the Ra223 herself.
The biggest concern was my bone marrow function. Without bone
marrow, we ll would not
last very long. I have had chemo, but that was over 2 years ago so
damage to marrow
has recovered a bit.
Now Pca loves to live in bone marrow where it grows fast. So if
not killed by any therapy,
it can destroy so much marrow we die from the effects of having
not enough healthy marrow.
If Ra223 is sent into bone marrow via blood stream, it goes where
there is a lot of calcium
traffic caused by Pca met, and replaces calcium. It does not
replace calcium elsewhere.
Now the Radium 223 is an isotope of radium that is prepared by a
nuclear process so it emits
lethal alpha particles a short distance and has a short half life
of 11.4 days.
This means that when Ra223 gathers at all bone mets, including the
smallest, it radiates the
Pca molecule DNA and kills the molecule, or prevents it ever
growing, and the amount of
healthy bone marrow damage is minimal.
Our bodies act in a continual clean-up mode of dead and damaged
tissues, so the small
amount of killed material is removed and disposed of, and the
radioactivity by then has gone
down to low levels.
Some Ra223 is also disposed of mainly via small intestine so the
side effect of Ra223 is
to have diarrhea and nausea. These side effects may / may not be
acute and are
supposed to begin within 24 hours of having a dose of Ra223. So
far, 48 hours after my dose,
I have no side effects. I may find I would not have many side
effects because there has been
good uptake of Ra223 into my bones and the radium may lose a lot
of its radioactivity
before its ever moved out of my body, and it may not irritate or
damage my body in the process.
Although my Psa is doubling in 1 month or less, all my other blood
numbers are not changing
much. The amount of bone breakdown by my Pca is not huge, and I
know from PsMa
scans that many bone mets are mutations of original Pca at PG,and
they may be making much
more Psa compared to very low levels of Psa made by original Pca
in PG.
In Dec 2009 at diagnosis I had Gleason 9, locally advanced Pca,
but Psa only 6, and this was found
to be inoperable at the time for attempted open RP in Apri 2010.
I was diagnosed at least 4 years too late and should have had a
first biopsy in 2003 when Psa
was < 3.0, and I would probably have been found to have Gleason
5 at PG, and
an RP might have been successful.
I would not have practiced "Active Surveillance" or worse,
"Watchful Waiting" which is medical
talk for "avoiding the problem".
Unfortunately in Australia, the medical system does not urge men
to have a full examination
with MRI and maybe biopsy when Psa reaches 2.5, so that by the
time they do get examined
the Psa is < 3.0. In men who are never going to have trouble
with their PG, Psa is 0.7 at 40yo,
and 1.0 at 60yo, and many men have Psa > 1.5 at 70. They may
never get Pca.
But for the 20,000 men who are diagnosed in Australia each year
with Pca, quite a number
have much advanced Pca at time of diagnosis and with high Gleason
score and high Psa > 100
and they have tried hard to avoid ever seeing a doctor. But I had
yearly Psa tests for 10 years
before diagnosis, and because my Pca made little Psa, it developed
into a monster and probably
spread to bones well before diagnosis. It grew very slowly, and
when ADT and other hormone
drugs were tried, they slowed down the growth of what was at PG,
lymph nodes and bones.
It was difficult to see that chemo was doing anything good, and
scans confirmed that view,
but Lu177 seemed to work very well for all lymph node mets, but I
have to ask "what
is the condition of my lymph nodes now?" Could the new bone mets
be spreading back to
other areas of body? I think it is possible, but PsMa and FDG
scans have not seen it yet.
I have to wait a month to review progress of the first dose of
Ra223 before I have a second
dose. Basically, a reduction of Psa rate of increase is at least
expected. When I had my first
Lu177, Psa stayed the same until after the 2nd dose. I expect a
similar response with Ra223.
And because Xtandi is now not working as it was designed to do, it
won't make Psa
reduce a lot and make the effect of Ra223 look better than it
really is.
Xtandi was added too late and after my 3rd dose of Lu177 in April
2019 to boost the PsMa
expression to make Lu177 work a lot better than without Xtandi.
Perhaps that occurred,
but there is no proof that it did for the 4th Lu177 dose. By the
5th and 6th dose of Lu177
in July and October 2020, Xtandi has stopped having any hormone
blocking action it was
designed to do, and nobody knows if it also stopped boosting PsMa
expression which made
it less likely to get a good image in PsMa scans.
There's a trial at St Vincent's in Sydney still going on now to
confirm that Xtandi can boost
action and effectiveness of PsMa scans and Lu177 treatments.
Theoretically, more Pca cells
would be killed with less Lu177 doses and before Pca mutated by
being stressed by Lu177,
but not quite enough to be killed by Lu177.
Continuing research at Peter Mac in Melbourne have found some men
who had very advanced
bone mets were able to have two repeat courses of Lu177 and its
given these men 5 years
extra life since they began in 2016. But that's a minority of Pca
patients whose Pca did not
mutate much and who had high PsMa expression in scans thus leading
to effectiveness of
Lu177.
It just was not known if Xtandi would help when I began Lu177.
Without any Xtandi, Psa would have reduced, but maybe down to only
2.0 after 4 Lu177 doses.
But it has been found PsMa expression often becomes low after a
certain number of Lu177
doses so that more Lu177 just won't do much.
This is why Lu177 is not always a miracle cure. The PsMa
production by Pca cells is very fickle,
and its sometimes there, sometimes not there, so LU177 or AC225
will work when PsMa is high,
but not when its low, so the mean time where Pca growth is stopped
and tumors are reduced to
a minimum and Psa has maybe returned to what it was at start of
Lu177 is about
14 months, which is about what I got, with 4 doses, but then all
mets and Psa increased and a
5th and 6th doses reduced Pca and Psa again, but nowhere near as
much as first 4 doses +
Xtandi did. New mutated Pca was seen in bones, so having more
Lu177 would be useless.
But at least the outcome from Lu177 was better than I believed was
possible from chemo,
which very often only works for awhile until cancer mutates to
resist the the effect of chemo.
I just don't know what outcome will be from Ra223. It might give
me months more life, or years
more, or appear to give big reduction of Pca and Psa, followed by
extremely fast increase of
mets and Psa which cannot be treated by anyone, and the medical
system becomes too slow to
look at DNA of the Pca, and choose the best drugs.
I did have blood DNA analyzed in November 2020, but I was Brca1+2
negative, and no genes
could be found to indicate there was any probability I would get
Pca or any other serious disease.
My mother lived to 98 without getting any major illness except the
weakening of old age, arthritis
and inactivity, and reluctance to ever exercize. My genes to get
Pca probably came from my
father's side of family, which had plenty of cancers as cause of
death before 60.
So I need to think outside the square and look at additional ways
to attack my cancer. The fight
should go on.
Some say that having a battle with cancer is silly thinking, but
then usually these ppl don't have
cancer, and if and when they get it they might think very
differently.
Chances are that nothing else works after Ra223 is done. I cannot
have an endless number of
doses because of accumulated ionizing radiation effects on bone
marrow. 6 doses of Ra223 at
about 6 weeks apart may be possible. That is 36 weeks or 9 months,
so I may have last Ra223 in
November 2021 with cycles ending in December. Ra223 has been
around since 2000,
and more good reports than bad reports about it may be read at
Healthunlocked.com.
4 February 2021.
Following a 5th and 6th dose of Lu177 in July and October 2020, my
Psa went from 30 before
July to 7 in about November. For these 2 doses of Lu177, I
continued with ADT and Xtandi, and
was given Veyonda, ( idronisil ) to take for 2 days before Lu177
and 8 days after. Docs said the
Xtandi and Veyonda boosted PsMa expression and increased the
quantity of Lu177 which is
held close to my Pca bone mets by means of the PsMa ligand
chemical.
A follow-up PsMa Ga68 scan last November 2020 showed overall
volume of Pca mets had
reduced by about 1/2, with some that had been fully zapped, while
others were still alive.
But a number of new bone mets sprang up which had a feint image in
scan with low PsMa
avidity of only 1.6, while others had SUV 10, but docs decided I
would not benefit from more
Lu177 because it would only work on a few live mets and not
on all the new ones with low
PsMa expression, so having more Lu177 was not allowed.
But not one met was seen in any organ or lymph node, except for
small amount in prostate
gland. This indicates that whatever Pca is in my PG now, it has
now become resistant to Lu177,
chemo, or anything else, and it will be a long term problem. Its
low PsMa avidity has not
changed much since previous scans, so its slow growing, but could
be spreading new mets
anywhere. Nobody knows what's happening there.
So since November 2020, my Pca wasted no time growing because I
believe the ADT is
entirely useless, and Xtandi is now also useless because I think
it stopped working back
in November 2019, when Psa nadir went down to 0.32, and then began
to rise fast in early
2020.
But the Lu177 + Xtandi had held down Psa for 2 years. After a
total of 10 PsMa Ga68 scans
so far, the last 3 have not shown any mets in soft tissues.
Now its February 2021, Psa is about 70 now, doubling each month,
and I have a lot of bone
mets which are growing up and I am negotiating with
Theranostics Australia to give me
Xofigo, Radium223, and isotope of Radium which is an alpha
particle emitting nuclide with
1/2 life of 11.4days.
This does not depend on PsMa expression and does not need a ligand
chemical, but is
attracted to wherever there is high Calcium traffic in bones, and
into bone mets where the
alpha particles can break down the Pca DNA better than most other
things known.
Very little Ca traffic occurs elsewhere so Radium is not attracted
to these non-bone tissues.
The alternative action would be to try more chemo, with
Cabazataxel, but no doctor can
tell me just what the efficacy would be, and from what I have read
about chemo and Pca
in bones, Cabazataxel has slightly better efficacy than Doctaxel,
which I found to have none.
Just take a look at updated Psa graph below. The chemo response on
Psa was awful.
and the scans at the time showed Pca progression, with now mets
seen.
If I went for Cabazataxel now, it may weaken me so much that I
could not have Ra223 later.
The mean time for extension to life time for Ra223 is 4 months.
This means I could get years
more life, or none. If Ra223 did kill all my bone mets that could
be seen in scans, what about
the mets that cannot yet be seen in scans? These are always going
to be there.
Its possible soft tissue mets will be seen later, and chemo may or
may not zap them, because
they may have different DNA due to mutations. But by that time, my
capability to have chemo
or any nuclide treatment might be zero due to having poor bone
marrow functions.
Unless there's some other therapy, this will be the time I would
be forced to put up the white
flag and surrender to palliative care, and "get my affairs in
order".
There's a possibility that if I zap all bone mets, and deal with
whatever is at my PG,
I get a good long holiday from having to fight Pca. We all chase
possibilities.
I have no idea of how I will be in a year.
But I am continuing to cycle 200km a week at very good speed, with
no symptoms of
Pca yet.
See updated Psa graph below..........
Latest Update on health concerns 15 October 2020.
My Psa is going down after having more Lu177, on 24 July 2020
and again on 2 October.
Psa reached 30 just before 24 and is now about 8.
I had PsMa Ga68 PET CT scans last July which did not show any soft
tissue mets, and some
bone mets had healed. But some had not, and they had grown back so
the only reliable
was to have more Lu177. The Psa dropped from 30 to 8.7 after 5th
Lu177 shot in July, a
good result compared to when I had first and second Lu177 shots
where Psa moved from
25 to 17. But this time I was given Veyonda, aka Idronosil for 2
days before Lu177 and 8 days
after with purpose to boost PsMa expression by mets and attract
more Lu177, thus make it
more effective. That idea seems to have worked. I am also still
taking Xtandi which I doubt
is doing any testosterone reduction, but may is also boosting PsMa
production.
Nobody knows what is really going on.
I will know more about effect of 6th Lu177 shot in weeks ahead.
But I don't see any remission
is likely, and may need more Lu177 next year. The number of Lu177
infusions I could have is
limited due to accumulated effect of radioactivity.
I may have Ra223 next year because my Pca is only in my bones at
present.
I am still able to cycle 200km a week regularly, so quality of
life is OK.
Weight has stabilized at 77Kg, and I have regained average bike
speed about same as last
year. Neuropathy effects in legs due to chemo in 2018 has further
reduced. The trouble I had
with small intestine adhesions to 2010 operation scar tissue has
resolved. But it could occur
again.
June 19 2020
The effect of having Lu177 in 2019 seems to have faded, and the
added enzalutamide,
Ie, Xtandi is probably not working now. Yet again I am back at
square one with my fight
with prostate cancer.
Meanwhile, I have no symptoms and I have been cycling 200km+ a
week at good average
speed considering I am nearly 73. Nobody over 60 has ever
overtaken me on my cycle
rides around Canberra for some years, even though I have no
testosterone in my body.
I have not seen my latest 7th PsMa scan last week but my local
oncologist has
already referred me to talk to doctor at Theranostics Australia,
so I probably will
have more Lu177 soon.
Psa graph from 2013 to 2021.
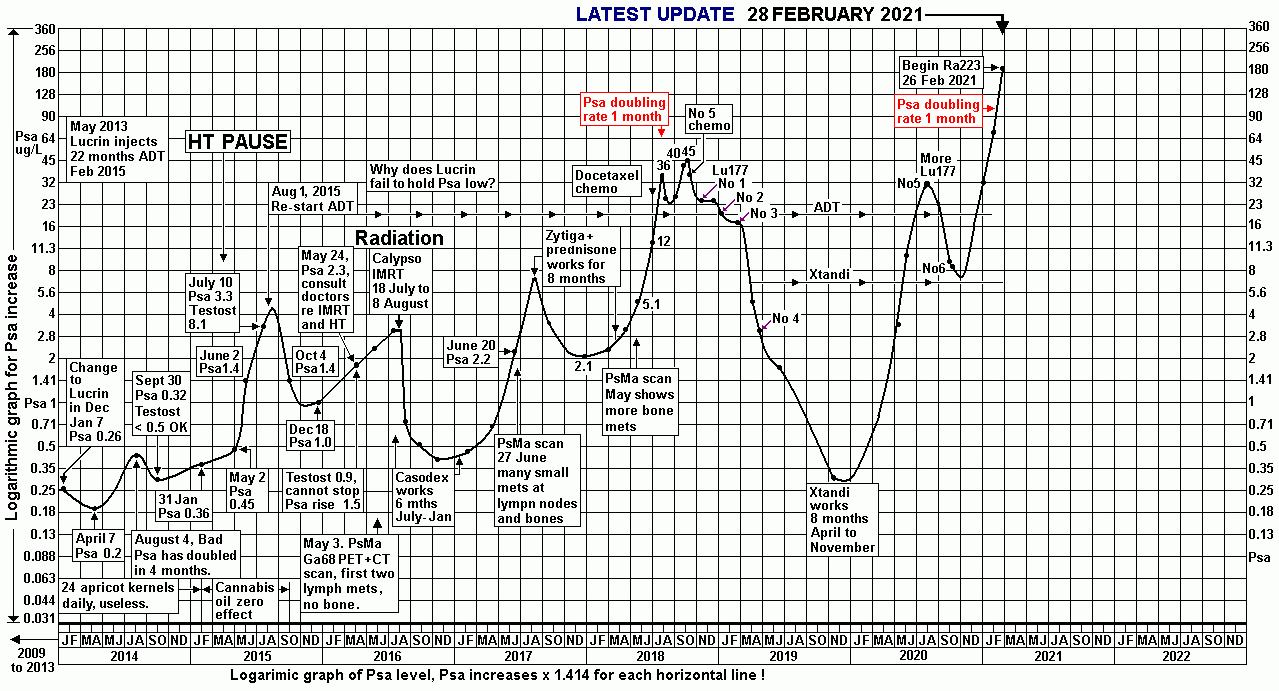
Up to 26 March 2020
Hi all,
I talked to oncologist today after Psa test 3 days ago, 23 March.
Psa has moved up to 3.5. It was at a nadir of 0.32 at 7 November
2019, and I estimated
doubling time of a month. So I expected Psa to be 0.64 at 7 Dec,
1.28 at 7 Jan,
2.56 at 7 Feb, and and 5.12 at 7 March, but rate has slowed a
little because Psa was
3.5 at 23March. Doctors don't know why Psa is rising, but not
enough rise has occurred to
justify taking any action now.
I did have full body and thorax CT scans 6 weeks ago where report
said 2 small bone mets
were one in L5 vertebra, and another in a shoulder blade. No other
mets were seen to be
active. But this activity alone may be enough to generate Psa of
3.5 now.
My oncologist was in favour of more chemo with Cabazitaxel,
slightly different to Docetaxel,
but because we have Covid19 crisis going on he did not want to
start me on the Caba,
because chemo reduces immune system function. I said I wanted more
Lu177 if Psa went
over 5, which it is sure to do in next 2 months, and Theranostics
Australia told me last August
after follow-up PsMa scan that I could have more Lu177 if another
PsMa scan showed it is
likely to work as well as the Lu177 I had during first 1/2 2019.
Meanwhile, life has been quite good but in late November 2019 I
had a small intestine
blockage caused by adhesions of part intestine to surgery scar
tissue formed after 2009
failed RP surgery. I was 82Kg when I
went to hospital, then I lost 8Kg in 11 days to be 74Kg, and since
then I have re-gained
3Kg, to be 77Kg, with less fat and more muscle. For awhile it was
uncomfortable sitting
on hard seats, or in a bath of water. But I am now back to cycling
220km a week and my
average speed is back up, and maybe some more muscle increase will
occur.
It is difficult and slow to regain lost muscle at 72 without
testosterone because ADT is
continuing. But I am not overtaken very often by anyone during my
cycle rides around
Canberra. Those who do ride faster are all younger with no cancer
treatment side effects.
Most days I feel 27, not 72, when I am on my bike. if I had bone
pains I'd be wanting to
get Lu177 asap, but I am OK now, and I have justified hope that
Lu177 will be there when
I need it in a couple of months without allowing Psa to get out of
control.
Recent research at PeterMac in Melbourne shows having more Lu177
is a good option
to kill off Pca that was not all killed off during first 4 shots,
or are new mets. It all depends
on scans. And I hope the availability of Lu177 is OK if Covid19
creates bigger demand
on all hospitals. if not, I could get Cabazitaxel but it is
dangerous for me.
But I have lingering side effects in lower leg function from the 5
shots of Docetaxel I had in
2018. I could perhaps get IMRT to treat the active mets if I can't
get Lu177, if there are
not many active mets, and they are able to be radiated with X-rays
without causing side
effects in organs within thorax.
It is possible the Xtandi is now not working to suppress Psa. I've
been taking it for nearly
11 months, and like Zytiga and Cosadex, these drugs don't kill
much Psa, they just manipulate
testosterone made by adrenal glands or by the tumor mets
themselves. Pca is notorious for
finding a way to prevent these drugs from working, and not being
able to be seen by our
immune system, and avoiding action of chemo or beam radiation.
Up to 13 November 2019.
My main recent concern has been my fight with Pca.
Last year I had chemo with Docetaxel which failed so I began
nuclide radiation therapy
with Lu177. I had 4 infusions between Nov 2018 and May 2019. I
also began taking
Xtandi pills after 3rd Lu17 infusion and am continuing with it. I
am also continuing with
monthly injections of Lucrin which are probably not doing much
because my body's ability
to naturally make testosterone may have completely atrophied by
now.
My Psa on about 7 November 2019 was 0.32, and it looks like it
will continue to reduce.
I have zero symptoms of Pca, and the discomfort of bone pains from
bone mets has ceased.
The last PsMa-Ga68 scan and the report showed all soft tissue mets
were undetectable
and while bone mets remained visible, they were not bigger, and
report says that healing was
underway.
Side effects from Lu177 are occasional dry mouth if sleeping on
back, or when
cycling at full speed for some time. Not enough to worry me. I
cannot notice any side effects
of Xtandi.
At present, there is no need for further Pca treatment but Xtandi
and ADT will continue.
I may have an Xgeva injection to improve bone density.
I stopped cycling over winter for a few months, then re-started
last August, and am now doing
over 220km a week at good speed for my age.
The damage to right hip I write about below was to muscle and
tendons from doing
paving work on house back in Mach 2019. I am not sure which muscle
or which tendons,
or whether membranes covering them were affected. Two doctors
thought I needed a new hip joint,
but an orthopedic doctor had a very close look and X-ray and MRI
scan and said problem
was with muscle and tendons as I suspected and not cartilage, so I
could cycle and should cycle.
I had already begun to get back to cycling a month before that
advice. There was only so much
winter rest I could tolerate, and whatever could heal was going to
do it within than time or not.
Seems like enough healing occurred. I had 20Grey of EBRT to my
whole hip area so the slow
healing was / is due to accumulated amount of X-ray beam radiation
I had to that area of body.
But so far, no acute pain at all when cycling hard on hills, not
even any discomfort while on a
long 80km ride, and none afterwards at night, so I guess the
cycling is helping to stimulate
healing. Side effects of last year's chemo were slow to fade
during my rest time, but once back
on bike my leg function has become better. My hands and arms are
less affected by vibration
when using lawn mower or hedge clipper.
Over winter, I was alarmed by weight rise while doing almost
nothing except living independently
and doing maybe average low amount of housework men of my age are
notorious for not doing.
So I became strict on carbohydrate and olive oil input and a
typical dinner was big plate of salad
with far less oil, 1 avocado, 3 fried eggs, and a pot of green
tea. Late night snack was a red pepper
and 2 tomatoes. Lunch was a vego sandwich at cafe, coffee, green
tea. That did the trick, no
more weight gain that is said to be a side effect of Xtandi,
especially with ADT continuing.
I have no central heating in my house because electricity prices
have gone through the roof.
Spare calories are used for heating me, not going to fat
stores to insulate me. So no pot belly.
So now after 3 months back on bike I have lost 3Kg and am 82Kg,
going faster, so its all
good for me, all blood numbers are OK and maybe I get to 80Kg by
Xmas.
As we age, many are an ideal weight at 30, but only if we have
worked physically and not
been a greedy glutton with calories or had mental problems that
disallow a person's
control over food intake. I was about 82Kg at 30, went up to 86
later, then 82Kg at 40 when
I took up racing on bicycles for 6 years. But I had a natural high
% of fat compared those who
won all the trophies in races. I basically have always been a
plodder, with no special athletic genes.
But at 72, and many years on ADT, there has been some muscle
atrophy, unavoidable for 90%
of men when they age, and become do-nothings. They may brag they
have same weight as they
were when 40, but fat % has much increased.
I found the benefits of staying fit and at my personal best gave
me fabulous sense of well
being and measurably much better health than all the other 72 yo
men around me.
They are rarely seen out cycling, and its years since anyone over
65 overtook me.
But my fat % has increased, and so as I age, I can afford to get
lighter, as both fat and
muscle masses decline. When I am 83.7Kg, BMI = 25.0. It can go to
23.0 if I was
77Kg, without bad health effects. I doubt my body will allow that,
because last time I tried it in
1988 my bike speed got slower on level roads with very slight
increase up hills. So I settled
for 82Kg when my 40km time trials were fastest, but still 5
minutes slower than many who
were older. You will just have to pardon me insisting I act and
think like an athlete.
Its makes many around me think I am odd, or unsocial, but all my
doctors think its wonderful
and I am the one who is putting real effort into staying healthy
and I don't need to be told
to lose weight, do more exercise and eat less rubbish, and get off
the booze.
Up to 15 June 2019.
I have completed 4 Lu177 infusions and 5 weeks after the 4th
infusion Psa has reduced to 1.6.
This is the same level as it was 2 years ago in June 2017.
The latest PsMa scan report from 11-6-2019 shows that my Pca
levels have been very much
reduced with virtually nothing in all soft tissues, and much less
in all bones, and there is no
need for a 5th Lu177 shot because it would not be able to achieve
much. So now I just have
wait and see what happens. I am continuing to take Xtandi, (
enzalutamide ) with Psa trending
down and I don't know how low the Psa will go, or how long it will
stay low.
My doctor said yesterday that if Psa goes up again then I might
need another PsMa Ga68 scan
and then have one shot of Actinium225, which usually works better
than Lu177.
If there was any sign of Pca which did not express PsMa then
perhaps I'd have a biospy of
bone or other mets to work out the best type of chemo to use.
Radium223 is also possible.
But the fight is not over.
Meanwhile, despite a painful right hip at night, and some walking
pain, I tried getting back onto
bicycle to ride 6km to and from a cafe where I have lunch. Well
that went OK for day before
yesterday but after today's pain free ride ride I had terrible hip
pains, My right hip has arthritis
and perhaps the thin or damaged cartilage was caused by the
primary Pca treatment back in
2010 when I had EBRT, ie, 70Grey of Xrays applied in 4 directions
in a cross formation to my PG.
The horizontal beams went through each hip joint. I protested at
the time, but the operators said
were no other beam directions possible. I probably was not
expected to be still alive now, let
alone wanting to get back to regular cycling. I suspect I have
radiation damage to hip joint
cartilage.
Last week one orthopedic doc I met seemed unable to explain
exactly what the
MRI and X-rays showed, and told me to come back in 6 months when
pain got very bad,
and then I'd have a 12 month wait for a new hip joint. Well, this
doc had done both knees
in early 2017, but he's retiring soon, so I will seek a second
opinion, and hope I get a
brighter doc of 40 who can read scans better, and explain each
sentence in a report.
The MRI scan report for hip mentions a cyst on a
tendon, and I have had these on my hands
from the electronics work using pliers et all in the workshop, and
these caused pains at night,
and they responded with cortizone injection to cyst, so an easy
fix might be available soon.
There's a big unresolved problem in my hip, and I will not try
cycling any more unless I get
answers. One problem with ppl having hip or knee replacements is
that they never recover
fully, and still have pains after their op. In my case, my knees
are now OK. But the hip may not
respond to treatment by replacing the joint. Many ppl whose DNA
ensures their cartilages in
knees to wear out may need hip joints as well, and I think I
probably am in that group.
I don't like pain killer drugs which have a pile of side effects
and numb the brain.
I have written a considerable amount about Pca at
https://healthunlocked.com/
Up to 7 April 2019.
The results of 3 infusions of Lu177 by Theranostics Australia
have led to a Psa reduction from 25
just before treatment to 5.0 now, and there's a light at the end
of the tunnel which does not appear
to be a freight train coming toward me.
Soft tissue mets have reduced to very low level in last PsMa Ga68
scans.
I am having No 4 LU177 treatment on 26 April. I have also begun
taking Xtandi, enzalutamide,
which my doctors tell me will increase the PsMa expression of my
bone tumor mets and make this
dose of Lu177 more effective than otherwise because more Lu177
will be gathered at tumour sites.
It is not known how long it takes to kill Pca cells after Aunty
Lutetia has shot up the Pca with her
Beta particle gun. The killing action may take longer than the 8
weeks between infusions.
But what's been mortally wounded will die, and nobody knows yet
what might survive to grow again.
Side effects of last Lu177 were slightly dry mouth for a weeks but
quite OK now. This time there
was very little ache in any bones where I have mets, some at about
the size of a pea. So far, doctors
think there is little challenge to the strength of any bones and
fractures are unlikely.
The descriptions of what happened before 7 April 2019 is in text
written for Jan 8 2019 below.
at the time.
But continuing on for this 7 April update....
Since before No 3 infusion nearly 6 weeks ago, my right hip has
become sore if I walk say
1/2 a km, then pain eases off after a rest and comes back with
another 1/2 km, so I have to slow
down to being like a 90 year old.
I have not cycled anywhere for about 6 weeks.
An MRI was done on hip, and two Pca mets show up clearly as two
pea sized lesions, one about
40mm above hip ball joint in pelvis and one 100mm below ball joint
in femur, and it is not known
if the mets are causing pain walking, due to the inflammation of
joint which can occur due to such
mets, small as they are.
I had a cortisone injection to the hip joint which seems to not
have done much.
I also had 20Grey of EBRT to my hip to hasten or assist the
killing of the two Pca bone mets near the joint.
That was only 2 weeks ago, and it takes time to become effective,
if it ever it ever is able to.
There is also a possibility of ligament damage near hip joint
which may be source of pain.
The MRI for hip shows I have serious cartilage wear in the joint,
ie, osteo arthritis, from a lifetime
of being active in building trades imposed on genetic bone quality
more suited to an office job.
Already one radiation doctor talked of a hip joint replacement
which could be given if the cancer
is put under sufficient control to suggest that its regrowth to
present levels could take years.
I am going to get an orthopedic surgeon to take a look at my hip
MRI, and read the report very
carefully, to establish what is really wrong, and get myself on
the waiting list for a hip joint if that
is really the best solution.
This time next year I may have been given the joint, before being
crippled between now and then.
Meanwhile, the two replacement knee joints I received at Calvary
Hospital are going very well,
giving me good mobility. My sister needed both her hip joints done
in her mid 50s, and my
Mum needed a hip at 86, and so she walked until just before she
died at 98.
Up to 27 May 2019.
The easing of pains in hip didn't last long and its not good and
pain at night stops a good sleep.
I am getting X-rays tomorrow and talk to a orthopedic surgeon in a
week. It will then become clear
just what might be wrong to justify having a hip joint
replacement. Meanwhile, I get pain in both
knee caps and perhaps the cartilages under knee caps have worn out
because they have had to
rub in the metal surfaces of the artificial end of femur which
would have a different shape to my
original femur ends, so I guess I have bone rubbing on titanium.
There are only a few sleeping positions which permit sleep, and I
need have a pillow under
right knee to prevent the pain in right hip. I'll see my
acupuncturist to show me which points to
rub to lessen pain.
Meanwhile I remain on enzalutamide and will have Psa test soon and
see my local doc to see what
Pca is doing. Knowing my luck, I would not mind betting that Psa
is now increasing, but yet another
PsMa a scan will be due in a couple of weeks to decide if perhaps
I need a 5th shot of Lu117 or
some other action taken.
So I definitely cannot cycle.
I spend 3 hours cleaning up in my work shed before doing another
craft project and the pains
lessened, but today I am paying in pain for my efforts, so a
complete day of rest.
Time is the Great Dismantler for all things on Earth. We wish
foreverness, but its an impossibility.
Up to 8 January 2019.
My last and 5th chemo infusion was on 11 October 2018. My
oncologist thought chemo would not
work and after 4 x Docetaxel infusions, he and other doctors
thought it was not working, so
he gave me a referral to the doctor handling Lu177 at Theranostics
Australia.
While I waited for the arrangements to be made for Lu177, I had
chemo No 5.
I have had two infusions of Lu177 in Sydney on 9 Nov 2018 and 4
Jan 2019.
Psa dropped from 45 at 11 October to 25 just before 9 November,
then to 21 just before 4 January.
The Psa reduction is not huge, and up to 2 weeks ago I have been
able to keep cycling without any
increase of slight discomfort in my cervical spine.
In fact, I cycled 960km in 3 weeks before 4 January. During some
rides I achieved average speeds
I have not seen since 2014, when I was 3 years younger and less
affected by successive cancer
treatments or by the double knee joint replacements I had in Feb
2017.
In general, side effects of Lu177 are far more tolerable than
chemo.
But during 4 days after 2nd Lu177 I have to reduce the cycling
distance because of slight pain in
right hip joint which occurs after 2km on bike, then it eases
down, and I can do another 14km,
so it is a bit strange. This new pain might indicate Pca is
progressing in bones, or perhaps the
Lu177 is actively at work in this area of bones and causing
inflammation in or around the hip joint.
Lu177 should now be active because it is still highly radioactive
and will be for a week or two more
before radioactivity reduces because of the short half life time
for
While LU177 is active, the alpha rays travel only a short distance
and radiate tumour cells as well
as some nearby healthy cells, thus causing some discomfort.
I am hoping that as the radiation reduces the area will become
less inflamed and pain will vanish
and I will be able to increase cycling distance.
I am not yet taking any prednisolone or other pain killers and my
doc did not insist that I do.
I do not want to provoke trouble in my body forcing myself into
cycling 90km in a morning before
the inflammation has subsided.
I found I can do many other things without pain, but the overall
effect of Lu177 has been more
tolerable than aches and pains of the week after chemo.
It is possible the Pca may have burst through bone surfaces within
the moving joint area and
such protrusion of hard matter can quickly mash up the cartilage,
and then I'd be crippled.
I know a couple of men who became bedridden and in hospital soon
after getting hip pain from
unexpected met behaviour hip joint/s, and also in their a vital
organs so they found themselves
with no idea what might come next.
I have ZERO idea of what the outcome of this Lu177 treatment will
be over coming months.
The first scans will be after 4th February, and if I get a good
Psa reduction and if scans show
reduced PsMa avidity in bones, then I might get good enough bone
health to continue cycling
without fear of wrecking a critical joint in my skeleton.
I have 3 enemies in this world, aging, treatment side effects, and
effects of Pca progression.
I have Psa less than 21 right now. I have reason to hope I gain
more time alive with good
quality of life. I have more hope than those with Psa of 200 or
2,000.
But I don't believe my Pca can be cured, or that remission is
possible. However, I may live
long enough to be treated by one of the new immune therapies or
nuclide + other chemical.
Much is happening in Melbourne including the Peter MacCallum
Cancer Research Centre.
11 October 2018.
Psa reached 45, then fell to 36 at 11 October, and so question
is,
"Is the darn chemo beginning to have an effect?"
I am continuing Docetaxel, but have begun arrangements to have
Lu177 Theranostic
treatments because Psa might not be giving real indication of Pca
status because it becomes
less reliable when bone mets are present.
But CT full body scans and PsMa Gallium 68 PET/CT scans show mets
in soft tissues of lymph
nodes have reduced and there is nothing showing in any visceral
organs, so I have a main big
problem of bone cancer. During 4th Chemo cycle I was able to cycle
on my bike at least 12km
for first week after chemo, and then go up to 60km before next
chemo. For last 3 chemos I
cycled 38km to-from hospital to get the chemo. There's a very
slight dull ache in cervical spine
which shows the most avidity for PsMa, so it has high Pca load,
and left alone, it will get worse
fast and give a bad pain in my neck. I am continuing to cycle
every day of the chemo time while
able, and side effects are minimized and I have a healthy diet of
lots of green vegetables.
21 September 2018.
Springtime is still cold with -3C mornings but now getting 17C
days.
But my Psa is now doubling each month after 3 chemo
infusions within 9 weeks.
After starting Docetaxel chemo therapy, Psa has moved from 12 to
40 in the 9 weeks.
The Psa "flared" from 12 to 36 in a few weeks, dropped to 26 to a
nadir of about 20, then
moved to 26, and then 40 on 1 Sep, and Psa is doubling now each
month.
I am having Neulasta 24hours after each chemo infusion to boost my
white cells, and
this has done a fine job without side effects. But the boost to
immune system has not
had any effect on reducing Psa or cancer so that AFAIK, my immune
system is helping
the cancer to survive and grow because it does not recognize my
Pca cells as rogue cells
which would otherwise be killed.
The high rate of Psa rise indicates chemo is having the
opposite effect to what was expected.
The flare of +300% of Pca after beginning Docetaxel occurs in
about 14% of patients and
indicates a lower mean survival time of 12.5months versus patients
with no flare who get mean
20.5 months, These mean times just as many get more or less time.
Your time may depend on
initial Psa at start and age and ability to cope with chemo side
effects and fitness, or whether
the chemo is any good at all, and in my case this seems true so
far.
My GP says the chemo has already failed. My Oncologist says that
if Psa continues rising at
present doubling rate of 1 month, and is say 50+ in 2.5 weeks
after having chemo no 4 infusion
yesterday on Sep 20, then the chemo will be deemed to be useless,
and no need to continue.
But if a miracle occurs, and next Psa has reduced on Monday 8
October, then Docetaxel may
be continued, but perhaps changed to Cabazitaxel, a slightly
different chemical.
Meanwhile, my Oncologist will find out what conditions are for
inclusion of a trial of either Cabazitaxel
OR Lu177. The details are at
https://www.anzup.org.au/content.aspx?page=therap
but it appears from what I read that its one or the other, and I
may have no control over whether I am
assigned to get Cabazitaxel, which I think will NOT work, or be
chosen to be assigned to have Lu177.
If I was initially assigned to Lu177, and it shows no Psa
reduction, I could not be transferred to
Cabazitaxel, and would have to complete Lu177.
Just what the protocol conditions are if neither of the therapies
work is unknown.
Therefore, I am going to ask to be seen by Dr Lenzo at
http://theranostics.com.au/
The range of treatments are listed at
http://theranostics.com.au/services/#TreatmentsAnchor
One other treatment offered is for Radium 223 which is more
effective for bone mets.
http://theranostics.com.au/radium-223-therapy/
All these therapies are not covered by medicare in Australia yet
and i could have to spend
a lot of money, which I would be able to find.
My cancer has cost Medicare about aud $200,000 so far, mainly
because the Australian
Medicare protocols do NOT require doctors to recommend to patients
that their prostate
glands be fully examined when Psa reaches 2.5, so that they get
examination results by
the time Psa is still under 3.0, allowing for delays in the
medical systems.
Had I had a full examination and biopsy of PG in 2005, when Psa
was lower than the 6.0 in 2009
when I had a biopsy, I bet some Pca would have been found, and my
Gleason score would
have been far lower than the Gleason 9 found in 2009.
During attempted open RP in 2010, Pca at PG was so advanced my PG
could not be surgically
removed. It was highly probable Pca had already spread to
thousands of places including my
bones, and only ADT has kept all the metastasis held low, but
these are all now growing rapidly
after anti testosterone drugs, Eligard, Lucrin, Cosadex and Zytiga
all have totally failed,
due to tumour mutations, or my body developing obstructions to
these drugs going where they
can be effective.
2 September 2018
Spring has just arrived, brighter sunlight, and it is lifting
the gloom of freezing winter.
But the beginning of 3 weekly Docetaxel infusions is a new form of
stress because its side
effects are not pleasant. I have had 3 infusions so far, and am
now on day 3 after the last one.
Psa "flared up", ie, went from 12.0 at beginning of chemo to 36,
then down to 26, and now it is
27, which may indicate it went lower over last 3 weeks and is now
rising to show chemo is
not working. But if it is not rising, it may be plateauing, ie,
settling at about 27.
This means the cancer is growing, but slowly. Psa measurement does
always indicate what is
happening with bone mets.
It is always depressing when I see the Psa doubling yet again. But
I have always known my Pca
may take me out. What is life without sadness? It is impossible to
avoid it.
I agreed with doc that we need to have at least 4 infusions and
another Psa test to see if chemo
is working, and whether I should seek Lutetium177 or Radium223
therapy which would be
available about 6 weeks after getting a referral from my
oncologist to to the radiation provider.
Jevtana, which is cabazataxel, is the next level of chemo and may
be tried to see if it works if
Docetaxel does not.
Side effects of chemo were many initial aches and pains which came
and went within 7 days.
After Chemo 1, white cell count fell from 4.0 to 0.17, within 7
days I had fever symptoms so I had
3 days in hospital on a drip for antibiotics for an infection
which was not identified.
I thought it was an infection in lower jaw from having taken 3 x
bi-monthly injections of Denosumab
for bone density.
That was too much, and because I have been on ADT for so long,
since 2010, the side effect
of Deno is lower jaw necrosis where the bone begins to die from
reduced blood circulation to
the jaw. It is strange that a drug to boost bone density causes
lower jaw problems in 1% of cases
where men have full testosterone, but where men are castrated the
incidence of jaw bother is
much higher, maybe 40%. The slight pain in rear right side of jaw
vanished after the 3 days
on antibiotics. But it slowly returned. The symptoms of lingering
slight tenderness indicates my body
is trying to get rid of a bit of dead bone, but the immune system
is not working to help the process.
6 days after Chemo 2, I had some strange pulsing pains in spine,
and more severe hypotension,
so dizziness after standing quickly. Then I had one day of severe
back ache where I needed to
use crutches to walk easier, but Pannadol Forte worked quite well
and pain went away in 2 days.
And since that time, 3 weeks ago, no more pulsing pains and my
heart rate has stabilized and
I think the side effects of Zytiga on my heart have now subsided.
I was given and injection of Neulasta to try to boost white cell
production after Chemo 2 and 3.
I have no side effects of that, yet.
I have had to reduce my cycling fitness activity. I cycled 270km
in week before starting chemo and
I felt very well.
But 9 days after Chemo 2, I began to cycle OK and I cycled 20km
over to hospital to get Chemo 3,
and got home fine.
So in 12 days up to Chemo 3, I cycled 100km so my body seems to
recover fast after the Docetaxel
levels have reduced to allow all fast dividing cells to begin to
get back to normal.
And during this period I could cycle up hills with heart and lungs
working as hard as possible and not
get the "pulsing back pains" I had had weeks before.
My doc says the chemo attacks fast dividing cancer cells even
though my cancer is a slow growing type
which seems strange because if it grows slowly, one suspects cell
dividing is slow, and not many
are prone to killing effect of chemo. Some cancers are easily
killed by chemo, but some are not.
But regardless of the theories, I have to try what is available.
At Chemo 2, I met a man in next Chemo chair along for a blood
cancer. we had talked briefly about
our bothers. His wife was also there, and yesterday, I met her by
co-incidence at a museum cafe
where she was waiting to meet friends and relatives to arrange for
her husband's wake.
He had fallen at home, broken bones around one eye socket, and got
an infection that went to his
lungs which just stopped working, so he died, all in 2 weeks.
So there is a huge risk where your immune system is severely
compromised; the antibiotics just
don't always work in this kind of case.
She'd remembered me talking to them weeks ago, and was all tears,
and I had to re-assure her that not
all was lost, she had a beautiful 2y0 son, was quite fit and
healthy, and responsive and loving, and hence
quite beautiful, so time would heal her, although it would be a
struggle. I'm 71, and wished I was 35.
We cannot be here forever.
18 July 2018.
I saw my dear oncologist today, and we both agreed the next
step is chemo, ie, Docetaxel,
which includes the refined chemical taxotere which is derived from
a Yew tree somewhere.
Psa has hit 7.8 last Friday, up from 5.2 just 30 days ago.
I stopped Zytiga last Thursday, no need to continue, it is now
doing nothing.
I begin chemo on 17 Jul, with an "education meeting" on 12 July. A
friend had the 3 weekly doses
for 30 weeks and it has now stopped working but while he was on it
he had few side effects
because he's under 60 and fit and healthy and played competition
tennis in the last week.
I am not sure what he will try next, but but there will b a time
when my chemo stops working,
and some Pca cells will continue growing, and then there are 4
levels of chemo offered
by Canberra Hospital. My doc says that many patients get a real
benefit from the next level
of chemo after having Docetaxel.
I can have LU117 whenever I want it, AND maybe radium 223, and the
wait time is about
"6 weeks" but that could easily be 8 weeks. I can wait to see what
the first few chemo doses do.
The chemo is supposed to affect fast dividing cells, Pca is
considered to be in that group but
that seems strange because Pca is a slow growing cancer, well, it
is in my case, compared to
some other fellows, one of whom has gone from diagnosis with "low
danger+ Pca to beginning
of chemo in 2.5 years. I had low-danger cancer back in 2005, but
was not diagnosed until 2009,
but then had Gleason 9+9 high danger Pca that was inoperable, so
I've taken 13 years to
get to the same point of treatment. I know another who has what
might be called "wussy" Pca
and no chemo yet, and diagnosis was 25 years ago in 1993.
Last May I had a PsMa Pet gallium + CT scan which showed more
bone mets than I had last
year but no more "PsMa avid" mets in my internal organs. "PsMa
avid" means the mets that
appear in the scan are generating PsMa and gallium68 is attracted to gather at any place where
PsMa is generated, ie, cancer sites, by means of a chemical called
a "ligand" which is able to bind
the gallium and cancer site together, and thus generate an image
in a PET scan.
Lu117 can also be gathered at cancer sites and while there, they
give off beta radiation that travels
only 1mm so healthy tissue does not get high radiation. To
understand this type of radiation,Google
Theranostic prostate cancer treatments or try reading the site at
http://theranostics.com.au/?gclid=CjwKCAjw8ajcBRBSEiwAsSky_bXb5jtpISEA7CFFwhefk2n0ISQZYactSTsHSjef8cgmg9eQy5ETkBoCqgkQAvD_BwE
I don't know what mets I have which do not generate Psa.
Almost all Pca cells generate Psa initially, but after they grow
and divide to make new cancer cells
they tend to mutate to become a slightly or greatly different form
of Pca which may not respond
to many treatments including ADT, RT, chemo and to added hormone
blocker drugs like abiraterone
and enzalutamide.
Pca may be eliminated from the PG, but if it has spread before the
initial treatment by surgery
or local beam radiation or brachytherapy, or it spreads soon
after, and RP or RT is done, then
a man is in Deep Trouble in the future because the spread cancer
will most surely grow to
threaten the man again, and again, after successive treatments. So
as time goes by, the man
may have lots of mets which do not generate Psa, and are resistant
to all forms of known
systemic radiation including Lu117, and all known chemo drugs, and
although Docetaxel is
thought by many to be fairly tolerable, the more powerful chemo
drugs will tend to slow the
strongest of men. There is a point where nothing at all works, and
even if Psa does not rise
much the cancer marches on and the lesions in bones grow bigger
and a man becomes
bed ridden and sick, and his happy time is over, time to say
farewell.
Just why does Zytiga fail? Nobody really knows, but its thought
that the cancer learns to
mutate to be able to grow while Zytiga is present. Chances are
that some Pca cells cannot
grow when fully deprived of testosterone, but some can, so they
grow and produce
increasing amounts of Pca.
At my June meeting with oncologist it was
decided I should soon move to chemo with Docetaxel and maybe
arrange for me to have
Lu117 injects which I think would be good for all my Pca because I
am not yet so very ill
and have Psa below 10. But the Lu117 may not have much effect on
bone mets, and I might
need Radium 223.
There was also talk of getting DNA analysis of cancer cells to see
what chemo would work best.
I will believe it when I see that the docs have referred and if I
am a suitable candidate for the very
latest treatments. Many men would have no possibility of such
treatment and they just get standard
Docetaxel and 95% die within 5 years after the first sign of bone
mets appear in CT scans.
Now I am faced with death, and the nest way to delay it needs to
be found.
There are now some advances with immuno therapy in UK where a guy
went from having 3
months left to remission like status because his immune system was
made able to recognize
Pca as the enemy. But such therapy is experimental, and does not
work for all men on which
it has been tried, and it is years away from becoming accessible
therapy.
I see my oncologist again on 3 July, and maybe things have been
arranged for me, or not,
and I can't know until then.
Up to 27 February 2018.
I'm still alive folks.
Since last July, my dear oncologist started me on daily Zytiga
pills, 4 x 250mg plus 2 x 5mg prednisone.
I have continued normal monthly Lucrin injections. I began the
Zytiga at beginning of August 2017,
when Psa was 7.2, and 1 month after ceasing Cosadex.
After 6 months my Psa reduced to 2.2 at end of last December and
doc was pleased, and said I might
get 2 years of Psa suppression. The median time for Zytiga
effectiveness is 10 months, just as many
men have Psa zoom up when Zytiga fails before 10 months and the
men who get a longer time of
suppression. I have no indication yet of how much more suppression
I will get before needing to
move to chemo therapy with Docetaxel and then qualifying to get
Lu117 systemic
radiation.
Today, 27 February, Psa = 2.3, so a slight rise. I have never
known Psa tests to be inaccurate.
I still have no symptoms of Pca. I feel 22 most days, and the only
discomfort is suffering bad postural
hypotension that started soon after 2 years on ADT, but which
seems to have become worse due to
effect of Zytiga which may cause low sodium levels leading to low
blood pressure, so that if I sit at PC for
2 hours, I am dizzy when i stand up. This is much worse in the hot
summer weather in my house with
no air conditioning, so I use the fans all day.
Instead of Pca symptoms, I have treatment side effects that are
remaining tolerable with same number
of night wake ups, virtually no leaking from bladder or bowel, and
continuing sexual mutilation which
always occurs where PG is highly radiated and ADT has continued
for more than 6 years.
Zytiga works to block the action of adrenal glands which produce a
low amount of testosterone.
This low amount is enough to allow Pca to live. But even with
perfect testosterone starvation, Pca
still remains alive, and nothing stops it slowly mutating to
something more difficult to treat as time goes
by. The Zytiga is supposed to stop the action / production of
dihydro-testosterone, DHT 20 times
more powerful than plain old testosterone, that is produced in the
slowly mutating tumours which
are responding to testosterone deprivation by things doctors do.
Just exactly what is going on in a man's body when he has Pca has
not been fully described and
is not fully understood and already I may have said things that
experts would disagree with, between
the times they spend disagreeing with each other.
I am not aware of one case of remission with Pca.
Plenty of men have had a Psa of say 100, or even 1,000, then begun
a course of drugs and Psa has
fallen to 0.1, and they are all tempted to think they are cured,
but no, cancer changes while asleep,
and sooner or later, the men are in despair until the next drug
does the same thing.
Charles Mack, a man I know in USA was diagnosed in 1992, and he's
now 85, and has survived 25
years after diagnosis. People like to read how he achieved that,
but his slow Pca progression
is what is called "indolent", so he's had time to adapt and think
about it and publish much material
about what most men and a lot of doctors need to keep in mind.
Survival for a long time after diagnosis is really just luck, and
most men don't get 25 years.
I have a friend in Melbourne who has gone from diagnosis to
beginning of chemo therapy in 2.5
years. He had RP, Psa went low, then soon went back up, so he had
IMRT to operation site at
Epworth just like I did in mid 2016. His Psa dropped, then rises
fast, so he was forced to accept
ADT but it only worked for a few months, and the addition of
Cosadex caused his Psa to rise
extremely fast, so the Cosadex seemed to encourage his Pca. His
docs decided his cancer was
not controllable by ADT or anything related to hormonal level
manipulation, so no Zytiga, no
Enzalutamide. He's had 2 sessions of Docetaxel and Psa has fallen
from 40 to 7 in 6 weeks after
2 infusions.
He's under 60, and got his weight well under control, is playing
competition tennis and is very active.
He has a wife and family who love him. So his live goes on until
it just does not, just like mine, or
yours, and how bad you feel about it depends on mental outlook
which varies, and I have seen
friends and my father, one sister all have to cope with leaving
this Planet.
I got back into cycling last June after having a double TKR just
over 12 months ago.
My knees now feel really good, and other arthritis symptoms have
reduced, so I can mow the lawn,
clip the hedge, and easily do enough housework to never ever need
assistance from a wife or
anyone else. I seem to cope OK without any partner so far.
I have cycled maybe 7,000km since June, and this last week I have
done 270km, despite some
hot weather.
In November I cycled with local Sunday ride group, see
23 Wanderers, http://www.pedalpower.org.au/rides-and-events/
But I found hot days were unpleasant so I rode alone for most of
December and January and
started at 6am, not at 8am the Pedal Power start time, so I get
home before 10.30am.
Temperatures are just beginning to go lower, and I will re-join my
group this autumn.
There was a cool Sunday last month where I averaged 25.4kph for
85km in hilly conditions.
Among the group of maybe 25, are maybe 5 men and one lady who can
of a total of 20 who
often get to the top of a hill before me. Although my knees with
TKR are good, they don't like
steep any more than the rest of me which feels reluctant to raise
heart rate to maximum and
endure the ride, rather than enjoy it. But these old dudes who are
faster up hill often cannot
keep up to me down hill and along flat roads so I manage to get to
the cafe stop first.
This activity will come to a grinding halt when my Pca gets worse
and if there are bad side
effects of chemo therapy.
I used to often average 29kph at age 61 on hilly country roads
north of Canberra with a full
amount of testosterone. If I still had testosterone I could expect
to average 27kph at 70.
But I can only average about 25kph, so the loss of testosterone
for many years plus my
plastic+titanium knee joints have doubled the normal loss of speed
due to age.
I really don't mind that what I was has gone, because so many
others are in a similar situation
and sometimes its good to cycle with a group.
To know how fast many older ppl can cycle, see the Age Standards
for UK
https://www.vtta.org.uk/standards
AFAIK, most time trial courses are on flat roads where fanatics
gather to see who is fastest.
I am not fanatic, I do not have a special time trial bike or
special clothing.
Doctors like to see me dressed in lycra, with a bike against a
wall near the waiting room.
My resting heart rate is 50 as I type this. They don't mind that I
have BMI < 25, and am fully
familiar with my problem with Puff The Magic Prostate Grenade.
There is still controversy about Psa tests being useful, and some
doctors say Psa tests are
a waste of time for most men. But I would be dead by now without
Psa tests, and even with
the tests, I was DIAGNOSED TOO LATE with Pca that was a very bad
tumour which made a
low amount of Psa.
I expect I probably carry Bca1 and Bca2 DNA which express
themselves as Pca in men.
Its the luck of the draw that determines your longevity, but
maintenance of a good frugal lifestyle
allows better coping with this horrible disease.
The graph shows clearly the effects of Casodex and Zytiga which is
somewhat common for
many patients and effects of necessary following chemo with
Docetaxel. Very seldom does
anyone see a Psa halving rate that has a time equal to the
doubling rate.
But back in 2013 and 2015 and 2016, halving rates were initially
fast, but always the Psa reduction
ceased and Psa went up again. Pca becomes resistant to all drugs
and radiation, and you can see
the typical Psa response as each new chemical is tried, and
eventually, there are no chemicals left to try.
Psa and
treatment history from beginning of 2009 to end of 2013. See
2014 to 2020 below.
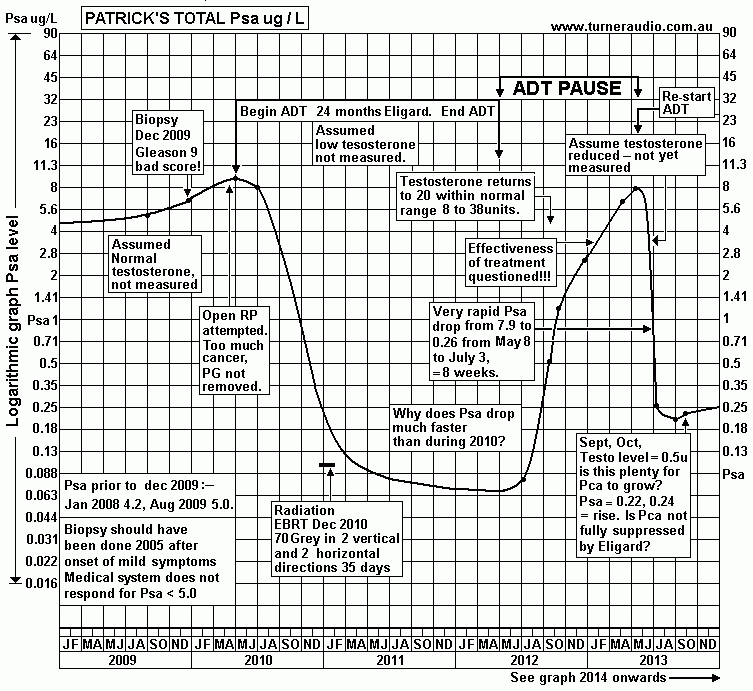
After some thought, I have concluded :-
1. All men should be able to have
their PG removed well before Psa moves above the
"normal range" between 0.3 and 5.5. The examination should include
MRI and biopsy at 3.0
for men who want it. For men without BPH or any prostate troubles,
average Psa is 0.7 for 40yo,
and 1.0 for 60yo.
2. The medical system of
Australia failed to protect me when it should have. I had regular
Psa tests once a year for 10 years before diagnosis. I got told
bullshit that they only think
action is needed where Psa rises slightly faster than normal when
its over 5.0. Have a biopsy
as soon as Psa goes to 2.5 !!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!!
Doctors may resist this request and I suggest you keep trying to
get what may save your life.
3. Digital tests, ie, a middle
finger up the arse by doctor often takes only 2 seconds. I don't
believe they tell a doctor much except that your PG is swollen.
One female doctor I had did
a digital exam in 2009 which lasted about 20 seconds and she felt
around in all directions and
she could only feel that I had a swollen PG which had no hard
lumps.
4. The Gleason score I got later was
9, with 9 out of 9 samples positive, and urologist who
does 100 RP a year said analysis showed aggressive cells, "young
man's cancer", and it then
took 4 months to the date for operation. My PG could not be
removed because there was too
much cancer outside the capsule. I should have begun ADT when
diagnosed.
I felt the Medical system had failed badly, so as a result of
their incompetent protocol, expenses
so far have totalled about $150,000, funded mainly by Medicare
with 13% from my pocket.
I can expect expenses to be another $100,000 before I die in about
4 years time.
5. If the Govt lowered the Psa
threshold to 3.0 for examining PGs they would have treated my
cancer early enough to get a cure. It seems to me that all men who
have Pca continuing on after
surgery have a long expensive battle until they die. Men with
inoperable cancer like me have the
worst prognosis. I was told that for Gleason 9, there was no
cure.
6. I would have had a Gleason 5
tumour well before 2009 when I was diagnosed, perhaps in
2004. As time goes by the tumour in PG mutates and its lethality
and Gleason score increases
so that men like me with Gleason 9 and inoperable Pca cannot
expect more than 10 years after
diagnosis.
7. I estimate I have far more
metastases than could be seen in my last PsMa Gallium68 scan
last June. The gallium68 scan is good, but cannot show small
tumours < 2mm. I guess many
mets began during last 10 years and some may have begun well
before diagnosis.
8. If I had been diagnosed in 2004
with Gleason 5, I could expect the RP op to spare my nerves
around PG which would have allowed continence, and erectile
function. If there had not been
spread, surgery with Gleason 5 would have been more likely to give
a cure. Without ADT,
extermination of my sexuality would not have occurred and I would
have had far better bone
density and a higher fitness level due to continuing testosterone.
------------------------------------------------------------------------------------------------------------
14 July 2017.
My prostate cancer is progressing, and last Psa on 20 June was
2.2, with doubling time of 2 months.
I began Casodex in July 18 2016, but it only worked for 6 months.
I have continued with Lucrin ADT.
I stopped Casodex 2 weeks ago, and my oncologist suspects it
promotes Psa rise once it stops working.
A PsMa scan in Canberra on 26 June found numerous metastasis in
upper lymph nodes in chest, and in
spine and other bones. I suspect all these mets have been there
since before I began treatment in 2009.
The PsMa PET/CT scan has detected all these mets about 3 years
before previous CT or PET scans
were able to. The usual prognosis once previous scans found bone
mets was 3 to 4 years of life, with last
year full of pain and not worth living. I am now pausing Casodex,
and Nilutamide will be tried, plus other
things after I see another specialist in Sydney with more
experience with Pca, and where there are some
trials of latest treatments.
Meanwhile, my knees have recovered after double knee joint
replacement last February, and I feel very well,
and have been able to cycle 200km during last 2 weeks and at
average speeds I have not seen since 3
years ago. Knees are still a bit stiff, but they are likely to
improve further.
I have read where doctors have said that when Pca begins, it
immediately begins to spread. And a man of
45 could have minute amount of Pca in PG, and then elsewhere, but
because Pca is slow growing, it may
be many years before Psa rises.
For men without any Pca, and unlikely to get it, normal Psa is 0.7
at 40 and 1.0 at 60.
If I had been examined in 2004 when Psa was 3.0, they may have
found Pca, a small pea sized tumour,
but it still may have spread to may places. So Pca looks to be a
much more difficult cancer to treat.
Men like to think their Pca in their PG is easily treated and then
its gone. Well why have all the fellows I
know who an RP operation get rise in Psa afterwards? Some had Pca
continue on near site of operation.
So they get radiation, and that's only 50% successful, and I know
fellows who had Pca continue after RP
and RT.
In my case, my Pca generated low Psa for the size of the tumour in
PG. So docs abandoned surgery
after opening me up, too much cancer. I was in the small number of
patients.
In July 2016 about 1 year ago, I had IMRT with Calypso at Epworth
Hospital in Melbourne.
This treated PG and the two lymph node mets they found during PsMa
scan. The recent PsMa and the
report says that the 45G I had to 2 lymph nodes may not have done
much, but that the 31G I had to PG
had reduced original PG tumour. This has allowed me better urinary
and bowel functions. But to really be
sure of killing a Gleason 9 PG tumour, Brachytherapy with 150Gy is
probably best. EBRT and IMRT
cannot deliver high enough radiation levels without damage to
surrounding organs.
So, where from here? Well, later this year, all the results of a
trial of theranostic treatment with Lutetium 117
at Peter McCallum Hospital in Melbourne will become published.
This offers hope, but side effects are
ruined saliva and tear glands. I heard there were problems with
liver and possibility of future leukaemia.
But the Lutetium 117 is targeted radiation, and it appears my
tumours generate enough Psa to be targets.
Where Psa mets do not generate Psa, there is no way to target
radiation or other chemo drugs which bind to
Psa where it is being produced. The timing for Lu117 treatment is
not urgent, because tumours could be
10 times larger and still be able to be treated. And then there is
the likely fact that although maybe 20 met
sites have been found, there could be hundreds of tiny mets yet to
be detected because they are so small,
and while so small, they have no effect on general health.
I was told there is some immune therapy being trialled in Sydney.
There was an article in local paper
about a young man under 40 with rare gall bladder cancer, and he
had immune therapy which appears to
have been successful but it cost $230 per day, or $84,000 per
year. Lu117 is offered by a Perth base clinic
and is $10,000 per treatment, and maybe 4 are needed over a year.
It will be years before such treatments
become mainstream in public hospitals, and health insurance may
not cover all costs. As you get older, be
prepared to pay huge amounts of dough to stay alive; its much more
important than buying a new car, or
making sure the grand-kids get big payout from your will.
The fact of life is that some underlying condition of cancer, bad
heart, bad lungs may exist at age 50,
and then take 30 years to cause death. I lost a sister from
ovarian cancer, and from symptoms to her
passing was 2 years. I had a customer get pancreatic cancer, and
he died within 18 months. The doctors
are not magicians or Gods, or miracologists.
3 June 2017.
In my February update I said :-
"""My Psa has risen from 0.39 to 0.45 over last 3 months which
shows that Psa is not continuing to fall and that
the radiation I had last July and continuing ADT with Lucrin and
with continuous Cosudex from last July was not
enough to stop the Pca from progressing. I have always feared that
last year's treatment would only delay the
inevitable and sure enough, Psa is now beginning to rise again
rising.""""
The Psa test was 0.7 on 10 April 2017, and it looks certain that
my prostate cancer is on the march again.
The graph applies to myself only. Anyone else may find that their
Psa levels and Pca history are nothing like
mine if their cancer cell type and treatment were very different.
The rise of Psa at far left side indicates Calypso IMRT radiation
at Epworth Hospital in July 2016 plus addition
of continual Cosudex since last July has not killed the cancer.
Before getting the additional treatment, last year I
suspected my cancer was radiation resistant, ie, it would take
perhaps 200Grey levels to fry the bastard to death,
and I have only had a total of 100grey to PG, and 45Gy to two
lymph node spots.
Cancer often defeats whatever doctors do, and not all cancer cells
are the same, and while some cells may be
killed by each treatment, others survive or mutate into something
harder to treat any further.
I think this cancer will continue to chase after me for the future
I have left.
My next discussion with my good oncologist in June 22 will have to
deal with my castration resistant Pca;
despite ADT with monthly injects of Lucrin, and addition of 50mg
of daily Casodex pills, ie, bicalutamide, since
last July, Psa is zooming up.
My last oncology consultation was with intern oncologist instead
of the specialist doctor on 13-4-2017; my
specialist was overseas. The intern said there have been some
improved access to new treatments.
My next Psa test is due 17 June. I expect about 1.5. It probably
will confirm the trend of rising Psa. But this is
still LOW Psa compared to many who were diagnosed 8 years
previously. A decision will be made about getting
another PsMa scan with Gallium-68. now available in Canberra.
I do not know if treatment with Leutetium117 is now available at
Peter Mac for $40,000 in Melbourne, but a
clinic in Perth offers it. Usually, you cannot phone to find out
about this sort of thing; all inquiries must be via
doctors, and at some cost, and always to ensure that the treatment
is appropriate and does minimum harm.
In other words, before being considered for Lu117, you need to get
over hurdles of "eligibility", which may include
having tried all other treatments and you are facing death soon. I
have not seen anyone recommend Lu117 to
treat early stage of Pca like mine, which is so far asymptomatic,
ie, I don't have symptoms of pain or multiple
metastasis, and there are no known cancer lesions in bones.
I heard LU117 was being trialled in Sydney, but I am not sure
where. My Psa graph indicates the present rate
of Psa doubling is 3 months, and the speed of Psa increase may
increase.
Since April, I phoned a relevant research doctor at Canberra
Hospital and no Immune Therapy is available in
Australia for Pca. I searched for BAT in Australia and it is now
only begun to be trialled in USA by research
doctor Sam Denmeade.
See the video at https://www.youtube.com/watch?=fwestwwRTUNo
I think I definitely qualify for Bipolar Androgen Therapy because
I am asymptomatic and have had ADT for
last 5 years which has probably made my cancer cells generate many
more receptor cells to accept testosterone,
so it can get enough to grow from the tiny amount in bloodstream
despite the ADT reducing. The adrenal gland
and muscles produce testosterone, and its impossible to completely
suppress all presence in any man. BAT
involves having repeated injections of 400mg of testosterone to
give a high level which does not last very long,
and this floods the much increased receptor cells in Pca, causing
trauma to Pca cells killing many cells.
Survivor cells regain their tendency to be sensitive to low levels
of testosterone so they shut down until they
begin to generate more receptor cells. Si it seems BAT can extend
the time that ADT is effective.
During months of BAT, Psa is measured. After a high level shot of
testosterone, Psa does rise, but then in
most patients Sam Denmeade mentions, it then falls rapidly, and
after a few such "cycles" the levels of Psa go
lower than at beginning of BAT. Some patients responded with Psa
becoming so low as to be unmeasurable.
One could say that playing with testosterone levels is like
Russian Roulette, but just what else do the doctors
have to offer me? It may be more aggressive ADT with Ezalutamide
and Abiraterone, or chemo therapy, but I
know where all that leads, a succession of Psa reductions then
failures, and the medicine cabinet is soon
emptied after one drug fails after another, and finally the Pca
spreads and flourishes and the side effects
of treatments become intolerable. Morphine begins to look real
good.
Since last August, bladder and bowels seem to have fully recovered
from last year's RT, and from a double
knee replacement last February. I have also been taking
daily Flomaxtra pills to try reduce PG swelling and
constriction of prostatic urethra. During the day when I am up and
about being busy and now cycling 100km a
week, I have good continence, and a good flow rate. But at night,
when sleeping, I am woken 6 times in 8 hours
to pee, but I go back to sleep within a minute or two. Being
horizontal and not active seems to cause bladder et
all to be a bit over active.
I suspect that that even though there are small amounts of Pca in
the lymph nodes, they would still require the
same very high amount of RT to kill the Pca cells. There isn't any
harmless way of delivering "pencil beam" X-rays
because even if tumours are small, the beams spread out to be much
wider than a pencil. This is the nature of beam
radiation; beyond the theoretical pencil beam there is damaging
radiation extending outwards 10mm to 20mm,
and radiation continues on to tissues beyond the target.
My doc said that the Lutetium 117 treatment can safely deliver
200Gy of beta to areas where Psa is being
generated, ie, to tumour sites, and and this most definitely
overcomes any "radiation resistance", and the beta
can only penetrate 1mm beyond the molecules of Lu117 held steady
by binding agent to sites where Psa is produced.
Trials of Lutetium 117 were underway on 30 patients with Pca at
Peter Mac last August, while I was in
Melbourne. A video was made of the treatment known as "theranostic
radiation". The video showed results on one
patient riddled with bone cancer and with months to live. The
initial results were nothing less than miraculous for this
patient. But I have now heard not all patients did well, and the
full results of the trial will not be released until later this
year, probably at least 12months after the last guy was treated in
the trials, so maybe we hear something official by
next October. Time is needed before announcements because the side
effects need to be followed up.
It seems that when Pca spreads, it sometimes mutates into a cancer
which does not produce Psa.
Therefore a Psa in a blood test may not indicate the activity or
the spread of the cancer, and that MPsa scans will not
show where metastasis has occurred, and Lu117 would NOT be
effective because it could not be delivered by
the binding agent depending on Psa as the target.
----------------------------------------------------------------------------------------------------------------------
Back in Early February 2017, I was able to ride over 200km a week
on my bike at average speed of 22.5kph.
I could still ride, but walking or working was painful for my
knees. Weight was steady at 83.9Kg, resting heart rate < 50,
and not many uneven beats. I was looking forward to having both
knee joints replaced on 13-Feb.
I had the operation on 13 February. I spent a week in recovery
wards, then 2 weeks in rehab ward at Calvary
Hospital in Canberra. If anyone is sick enough to have to stay a
long time in hospital, then Calvary is The Best place
to be. Their ethics are excellent.
The first week was painful and I was allergic to Endone. I was
changed to Targin based pain relief for a total of 5 weeks.
I gave up using crutches at 8 weeks after the op. I had my first
bike ride of 6km on 22-4-17, and I felt I could have
ridden further. I modified one of my bicycles to have 160mm long
cranks instead of 175mm cranks to allow pedalling
with much reduced maximum knee bend. The main problem after TKR is
getting enough knee bend and getting knees
to straighten.
Being able to ride most road bikes depends on minimum angle
between femur and tibia to be less than 80 degrees.
I can only just get this with R knee. L knee has more bend, and it
is more comfortable pedalling than R knee.
I guess I will improve over time.
I lost over 3Kg in hospital because of the pain medications and
hospital food, which is sufficient for survival, not
wonderful. The Targin plus other drugs are fairly toxic to bowel
function and probably exterminate many of the gut
bacteria essential for good health.
From week 3 to week 8, I slept very poorly at home and was slow to
regain weight. But 2 weeks after quitting Targin
and have put a Kg back on. I was sleeping better week 9, not being
woken so often by pains. I went back to diet of
mainly vegetables with less than 100gm as of carbs or protein a
day. It is The Only way for me to stay well fed, keep
weight constant and below 83Kg.
I just had to learn to walk ride a bike again. At week 9, I could
walk 1km+ without crutches.
I am now at week 14, and have continued to improve walking and
cycling. I walk about 1/2 km daily just getting
around to care for myself, and I've been riding 100km a week; a
typical ride is now up to 22km, on mainly flat roads
with gentle hills. The bike I have been riding is a single speed
bike with 44t chain ring and 18t freewheel cog on wheel
which gives me a 65 inch gear which I am pushing this with 160mm
cranks so the gearing at low speed feels the
same as the 72 inch gear with the 170mm cranks I used previously.
This gear is a bit high for me at age 69, but I just
slow down and try to concentrate on turning the pedals right
around the circle. But after riding say 18km on 5
consecutive days, my knee-caps get sore, and I need to take 2 days
off bike and I am then better when I return to
the bike.
I have also spent time restoring a second bike with a nice frame
using Reynolds 531 tubing. It has old Shimano 3S 3
speed hub gears from a 1980s ladies bike which was not ridden very
far, and in good condition. It will have about the
same top gear as I push now, but will have two lower gears which
should allow me to ride anywhere in suburban
Canberra, with concentration on pedalling quickly with low stress.
I should be able to turn the 170mm cranks OK.
I hope to be back on my 10 speed Cannondale with 175mm cranks
within a month or two. The rate of increase of
knee bend is like watching a glacier move along a valley.
---------------------------------------------------------------------------------------------------
Maybe my knees will get nicely better just in time for the cancer
to pull me down again.
But I ain't no quitter, and I will seek whatever other forms of
treatment are available. I see my GP in 2 weeks and
oncologist in 3 weeks and will ask them both to find out what is
now possible in Canberra or in Australia.
Being positive for me means understanding all the negative
possibilities while sensibly taking action to extend life
to the maximum. I cannot live forever.
----------------------------------------------------------------------------------------------------
Prior to 6 February 2017, I wrote.........
Weather has been succession of heat waves with over 35C, and some
hot nights making it impossible to get to
sleep before 1:00am.
25 November 2016.
The spring weather has been delightful and my overall condition
has improved. For newcomers to my blog here, I had
an additional 31Grey of external beam radiation therapy applied to
my prostate gland from July 18 to August 9 this year.
This added to the initial 70Gy I received in 2010. Thus total RT
to PG was about 101Gy. Severe radiation colitis
occurred from August 20 to about October 30.
Side Effects. But since October, the radiation colitis symptoms of
enduring high flatulence and 8 daily toilet sessions at
least has eased off and bowel function has become closer to
normal.
The result of RT has mutilated my sexual function. For those not
used to the unpleasant facts about prostate cancer
treatment, let me explain :-
All men I know who had an RP have had complete ED. One man told me
his wife could excite him to an orgasm
without a hard-on. Maybe she sucked patiently, or more likely used
a vibrating vagina toy with suction. He could not
go into details with me. Too many male inhibitions about sex
details. Toys are NOT like the real thing, and probably
most ppl over 50 would just give up wanting sex, and complete
their partnered life without sex.
But I estimate more than in 50% of partnered relationships where
there has been no disease of sexual organs, the
couple have ceased having sex. Nobody ever admits it though. A
small % of women would seek real sex with a
whole man elsewhere and maybe get a divorce. For those who had an
RP, and no ADT, desire remains because
testosterone remains. But of course most older women's desire and
ability to have sex rapidly dies above age 50 or
earlier, so a man of 60 wanting to do things is irrelevant. He
cannot even jerk off. All men I know who had an RP
found Pca returned and they needed a full 70Gy of PG radiation. I
know a case where one guy had the EBRT a
year after the RP, and 18mths later his Psa began doubling each 2
months, and he is in SERIOUS TROUBLE,
and will probably need to start ADT and consider whatever else he
can get.
I believe these sorts of Pca troubles are far more likely than
doctors like to tell you, or more likely than publications
from Cancer Councils and other Govt advisory bodies.
I did not have RP, and had RT and ADT as primary treatment, and
after 5 years at age 66, I suddenly got
fibroids in erectile tissue, and Roger shortened by 30%. This is
said to be a direct result of prolonged time on ADT.
Erections are possible, but it just points down, is ugly, and is
useless for sex. There is no sensation of pleasure, and
no ability for the build up and release of explosive orgasm.
So, after Pca treatment, a man has to farewell his sexuality. Suck
it up Bro ! There are not many women enthusiastic
about a nice black strap on vibrating dildo.
Despite the chemical castration of ADT, desire for company of
women remains strong, and I enjoy talking to
those willing to talk. But many of the women I see around are
quite allergic to men after their menopause,
especially if they have been divorced. A really good relationship
with a partner should not rely on sex.
Urinary incontinence has never been a problem for me and I am
still OK now. It is due to fail at some time
due to RT damage to nerves. Fecal continence is OK, but when I
feel I need to go, I need to move very quick,
I cannot just put it off for an hour or two.
The PSA graph shows the fall of Psa after RT last July to a nadir
of 0.39 last November. I have not had such
a low Psa since beginning of 2015. I am continuing with monthly
injections of Lucrin and daily Cosudex
and Flomaxtra tablets.
It is still too soon to say I got much benefit from IMRT at
Epworth Hospital in Melbourne where I received the
Calypso EBRT during July. I would argue it is impossible to say
IMRT did any good, while doctors there would
always disagree with me. I prefer evidence based medicine. I
believe the Cosudex is the main agent acting to
blockade whatever tiny amount of testosterone is in my body which
is not suppressed by Lucrin injections
once a month.
However, it is surely certain that RT at Epworth plus the RT I had
at Canberra Hospital in 2010 has done my
stubborn cancer cells no favours.
It remains to be seen if my Pca survivor cells which remain after
treatments so far will survive or whether they
become more difficult to treat in future, and begin to dominate
remaining radiation affected tissues, and then
spread or become some other form of cancer which may not produce
Psa and hence not be detectable by
Psa tests. There are a number of future possible outcomes which
all are quite awful.
I recently read a frightening opinion by well informed medicos
about Pca where one doc said the Pca can seed
itself in bones and then come alive some years later. More reading
indicates that once bone metastasis has
begun, and is detectable, it means you have only 3% chance of
being alive 5 years later.
I do not really know my cancer status; the more one reads, the
more certain I am that I am uncertain.
But between now and when Psa could measure 50 may be 3 years.
But right now, I am well enough to have a big knee operation and
put up with the battle it will be to recover
and learn to walk without pain and ride a bike a bit further -
before I die, so I can get married to suitable woman,
finish projects, get affairs in order, and leave much less mess
behind me than do so many other ppl when they
finally die.
I am booked in to attend a pre-admission clinic on 13 December in
advance of having titanium and
plastic inserts to both knee joints some time after January 2017.
--------------------------------------------------------------------------------------------------------
Before 20 October 2016 :-
Nothing much has happened to my health in the last month, except I
am still suffering effects of radiation
colitis, a side effect of having had radiation of PG in July. So
bowel habits are very irregular because the rectum
now cannot do its store before dumping routine which everyone else
takes for granted. The condition has very
slightly eased over last 3 weeks. I am now seeking a bone density
scan, and an injected drug to slow down bone
loss due to ADT which is continuing with monthly Lucrin and
Cosudex. Sleep is irregular, with 5 get ups a night,
and some nights I sleep less than 5 hours. There is no acute pain
and continence is still intact.
Before 24 September 2016 :-
My Psa was 0.52 at 24 September, going down from 0.73 at 17
August, and down from a peak of 2.8
in mid July 2016.
Why did this happen?
In Early July I went to Epworth Hospital in Melbourne to have
"salvation radiation therapy" using Calypso
IMRT applied to my PG and to two lymph nodes in upper thorax.
31Grey was applied to PG to raise
the 70Grey level applied in EBRT in Canberra in 2010 to a total
accumulated level of 101Grey.
45Grey was applied to each lymph node. There were two hospital
visits before IMRT on July 1, and
July 10, with IMRT applied twice a day from July 18 to August 9 to
PG, and once a day to lymph 2 nodes.
July 1. I had a minor operation to install 3 x RF beacons to PG to
guide the Calypso IMRT to PG.
A hydrogel pad of about 10mm thick and 50mm dia was inserted
between my rectum and PG, to push
the PG away so that high intensity X-ray beams did not fry a
section of rectum tube. In previous EBRT
in 2010, no hydrogel was used, and the amount of RT used on PG is
limited by what the rectum can be
allowed to withstand, plus other areas.
The Calypso IMRT has multiple beam directions, not just the 4 of
standard EBRT, and the path of
beams can be chosen to avoid areas previously radiated or those
where little radiation could be tolerated.
The radiation beams are not fine beams with sharp boundaries but
have diffused beams like a torch light
shining. But where all the beams intersect at the target, the
accumulated radiation intensity may be 50 times
higher than somewhere only 20mm away.
July 10. I was "measured up" and a temporary body cast made with
some sort of plastic-paper foam to
allow easy and accurate body alignment while on the radiation
table before radiation. The body cast is
not an enclosing cast; it is only 75mm high to wrap around the
underside of a body on a flat table, and
the cast allows easy body alignment by at least two staffers
attending before RT sessions began.
Tiny tattoos were placed when information from previous CT scans
was correlated so that for each session
of RT, my body could be positioned to within +/- 1mm of the
correct positions with laser light beams.
It is important that the huge radiation gadget knows where to aim
- guided by the tattoos and the three
"radiologically opaque" beacons which had been inserted to my PG
on July 1.
I began taking 1 Cosudex pill daily, each 50mg. I was already
under influence of previous Lucrin injections.
I also began to work on my bowel to ensure there was no gas or
shit in rectum before 9AM. That meant
continuing my vegetarian diet, but using one Coloxyl tablet each
evening to ensure a good shit by 8:30am.
It was important that I attend all radiation sessions shit&gas
free and with a nearly full bladder to keep the
PG in the alignment position as accurately as possible.
July 18 to August 8. There were 2 sessions of RT per day, 6 hours
apart, with PG and two upper lymph
nodes done at 10am, and PG again at 4pm. A Psa test was done on
July 18, but I was never told what
the result was, but I estimate it was 2.8.
My Psa rapidly reduced from estimated 2.8 at July 18 to 0.73 on
August 16, about a week after finishing RT.
The RT doctor forecast that Psa would flare up before reducing,
but that has not been observed.
By 24 September, Psa fell to 0.52.
I do not think the radiation has caused or assisted the Psa
reduction, unless this is proven to be the case
in future months.
The RT could only be deemed to be effective if I stopped all ADT
and the Psa continued to fall. I am not
going to stop ADT.
I do think the Cosudex has caused most of the Psa reduction,
because whenever I was previously given a
month with daily Cosudex pills, 50mg, there was a rapid Psa
reduction, as shown on graph.
I cannot say yet if the large expense and trouble of attending
Epworth has resulted in any worthwhile
benefit. Medical outcomes after procedures are often very
uncertain, and radiation effectiveness is still
quite low.
The full answer of what my Pca status is cannot be known yet. But
I have had Pca since about 2005,
with diagnosis in late 2009, with Gleason 9, aggressive cells. The
treatments and dealings with doctors
has made me very cynical, and I doubt many things doctors say.
After seeing that so many things doctors said were just
"Blatherations of Bullshit", I am sure many of
you now know why I am so doubtful about doctoral forecasts and
predictions. No doctor can be assumed
to be honest until time proves him/her to be have been truthful.
(( There is a huge disparity between what
many well trained, well educated, and obscenely paid professionals
say and what happens later after
prognosies have been given. But this is REAL LIFE, and what else
is there? honest fools? people who
had no idea? at least doctors do know more than one who'd trained
in 1716. ))
I was told in 2009 an RP operation would be fine, but that idea
was abandoned during attempted surgery
in April 2010. I was put on ADT, and had EBRT in late 2010, and
told "this will fix you!", but in 2012
I found the RT had been quite useless, and could have been
predicted because the REAL rate of RT
success with Gleason 9 is only a lousy 10%. ( Report from St
Vincent's Hospital Sydney )
After 2 years of ADT, I paused ADT in April 2012, with Psa <
0.08. But by May 2013 Psa went to 8.0,
and I was forced to re-start ADT. Doctors were WRONG about what
they said would happen. It seemed
EBRT had done nothing to halt my Pca. Psa went down to 0.2 after
ADT was recommenced, not as low as
before I paused. I has another ADT pause during 2015, this time
the doctors didn't forecast anything;
I thought, maybe good, maybe not good, and sure enough, Psa shot
up, and I re-started ADT. But the Psa
didn't go as low again and it began to rise while on ADT at
beginning of 2016. This seemed to indicate
typical ADT failure where Pca refuses to stop progressing even
with testosterone suppression.
But testosterone was 0.9 last February, and higher than the
recommended maximum level of < 0.5 to
starve a Pca tumor of testosterone on which it depends to grow.
Was the Lucrin having difficulty closing down testicular function?
It seems like it was. The addition of Cosudex
( bicalutamide ) to ADT with Lucrin starting at July 10 may be
doing the main part of good.
The monthly inject of 7.5mg Lucrin is easier to take than the
22.5mg for 3 months. Costs are the same.
By April 2016, the doubling time for Psa rise became alarming. My
good local oncologist said I could go
Epworth Hospital in Melbourne to have a new type of scan, the MPsa
PET gallium68 scan which has become
available in last 18 months. I qualified to attend Epworth because
my Psa was between 1 and 4. Epworth
had recently imported the Calypso IMRT method from USA.
On May 2, I had the Mpsa PET with gallium 68 at Bridge Road
Imaging and results were viewed on May 3
with the director of Radiation Oncology at Epworth Hospital. I had
an enlarged PG, and scan results showed
two distant spread spots in two upper thorax lymph nodes
"associated with the prostate gland." The doctor
said the spread spots were not in lungs or other organ. He said
these small level spots would not kill me
because I would have much bigger problems with the main primary
tumour within 2 to 5 years. Ah, so without
his RT, I'd last only 5 more years max. My PG tumor is ageing, and
probably began in 2005, but didn't make
a big Psa, so it was 2009 when Psa rose above 5. Old PG tumours
can end up being deadly. I have no idea
when the spread to the two lymph nodes occurred, but the doc said
the lymph node spread was a tiny amount
of Pca. Hmm, and I just thought, "from little things, big things
grow!"
The doc said he could offer more "salvation" radiation via Calypso
IMRT to increase accumulated level in
PG to a threshold more likely to cause Pca cell death. He was not
sure if it was possible to radiate the
lymph nodes at the same time.
I returned to ACT, booked appointments for second opinions for
which I had to wait a month. This gave me
time to search online for anything I could find about trials of
salvation RT for patients like me who had RT as
the primary treatment. I found very few cases where the PG was
radiated a second time after Pca began to
progress.
I was in a tiny minority category of patients.
I considered having a surgeon remove my bladder, PG, and seal off
penile urethra well away from outlet from
PG, having both ureters brought to a stoma, then facing life with
an external piss bag. The urology surgeon
who first saw me in 2009 was not interested in this surgery for me
at any time in future despite having done the
same thing for a friend of mine, and who has no Psa, and probably
no Pca cells in his body, and he is doing well.
But my friend accepted his op because he didn't want RT or chemo
etc, and the usual long drawn out and losing
battle. I'd been radiated, and the bigger op was now not possible
- too much danger of bleeding to death.
The most common op is to remove PG and join penile urethra to
bottom of bladder. It is the Radical Prostatectomy,
RP. It might be OK where Gleason score <6, but distance from
surgery to Pca is less than 20mm, and in many
cases the surgery area develops Pca. Therefore many who have an RP
will need to have RT and then have a long
battle to keep the demon of Pca under control, they may need the
years of ADT and chemo therapy; the fight is
never over until the cancer wins.
The surgeon said he might install a supra-pubetic catheter if my
prostatic urethra became constricted. It involves
a plastic pipe with balloon at end inserted below belly button,
and direct to front of bladder. The balloon is expanded,
has holes in it, and piss flows to a collection bag. But insertion
point is just above the vertical pathway for radiation
to PG which was done in EBRT. The holes for catheter insertion
heal up rather like the cells around a thick ring or a
bone which some ppl may insert through their nose or an ear lobe.
There is always a risk if infections.
My GP has a patient who has had an S-P-catheter for years, but for
other reasons than mine. It is the cheap easy
alternative to the stoma and bag to side, but the PG remains with
its Pca liable to grow and kill.
He did say I could try the Melbourne IMRT Solution, and getting
upper upper lymph nodes radiated in the same
sessions as for PG. I knew that he knew he could not help me much
in future, and I felt he didn't have much hope
for my long term survival because of what he found in 2010 when he
found he could not remove my PG - too
much cancer. He didn't ever tell me that. But what other
reason was there? I also I sought opinions from my
oncologist, and from the radiologist who did my EBRT in 2010.
None of the these three doctors in Canberra had the specialty
training or the software which could allow them to
view the 3D MPsa scans I saw at Epworth with the top radiology
doctor. The Bridge Road Imaging service
supplied a DVD with scan info, but it didn't include the
IntelliViewer software so nobody at Canberra Hospital
could view my scans any better than I could on a PC with Windows
XP, 7, or 10.
The latest gallium-68 scans give Pca patients and doctors with a
much better idea of the cancer status. Without
the gallium-68, (or choline-II in USA), it is difficult to choose
the best battle strategy. My scans showed metastasis
(spread) some years before any CT scan could show. And by the time
Pca shows up in a CT scan, its usually way
too late for treatment to be effective. If there were too many
spread spots then the use of any IMRT or EBRT
may be ineffective because so many beam pathways would be needed
that total amount of radiation applied will
cause intolerable side effects and damage to healthy tissues. Many
small tumors mean indicate systemic nuclear
radiation or chemo therapy et all may be better. Trials of
systemic radiation with Lutetium 221 are underway at
the new Peter McCallum Center in Melbourne.
Trails of Actinium 225 have been done in USA. The radioactive
element is in a solution, like salt in water.
There is also a secret binding agent that is specific for a type
of cancer in solution. This clear solution is pumped
into a vein or artery and during the next hour or more the
solution reaches all parts of the body. The binding agent
binds to tumor locations and brings the radioactive gallium ions
with it, and and magic happens; the tumor gets
a lethal dose of RT. While the radioactive ions circulate in the
blood circulation network, they don't linger so their
radiation dose to healthy tissue is negligible. This all gives a
theoretically positive outcome, but is somewhat subject
to many variables and laws of chance, but a success is deemed
where more than 50% of patients gain many years
of life afterwards.
But the most sensitive scans cannot show what will happen in my
future if I am already riddled with small amounts
of cancer spread which are too small for today's Mpsa scanning
methods to detect.
If I had the same MPsa scan in 2018, it is highly possible other
metastasis sites would be found, even if all the
metastases and the PG itself had gone into remission. There can be
a point where one chases an increasing number
of targets all over the body again and again with increasing sense
of futility and increasing expense.
Epworth Hospital must have invested heavily in bringing Calypso
IMRT and Mpsa tests to Australia within
last 18 months. Epworth is a "private hospital" which means they
charge exactly like wounded bulls, to ensure their
income from patients pays for the investments and returns a
healthy profit to those entitled to such profit from
business. The Australian public hospitals are often starved of
funds for the latest equipment available.
Following the month long pause to think, I returned to Melbourne
at beginning of July to proceed with the
Calypso IMRT for both PG and 2 lymph nodes. I signed what had to
be signed, giving verbal uninformed
consent because the doctors could not answer all my questions.
The proposed PG salvation radiation was to be done exactly the
same way as in vented by one Dr Gary
Shultz in USA. in 2011, The American Journal of Clinical Medicine
published an article about Gary's and its
easy to Google, but there are no records of any trials or patient
records to support Gary Shultz's claim in
AJCM that remission occurred in all 45 patients he claimed to have
treated.
These patients had previous EBRT which had failed stop the Pca.
Gary's technique is to apply an extra
31Grey to PG with continuing ADT and blockade ( Lucrin + Cosudex
). Calypso IMRT was less damaging to
surrounding body than the standard EBRT so the target radiation
level could be increased by about +50%.
Only brachytherapy with many radiated inserts could deliver more
radiation to a PG than any external beams.
So, Gary's treatment seemed TOO GOOD TO BE TRUE. I have no idea if
Gary treated 345 patients and had
45 successes, while not mentioning the other 300 who may have died
since 2011, suffering numerous tragic
side effects and recourse to other futile treatments.
It was not unreasonable for me to ask a professional radiologist
that he provide evidence for the likelihood
that what he proposed might work. I was forced to swallow the idea
that there was no real evidence that the
Gary Shultz method worked at all, and maybe it was no better than
the EBRT treatment I'd already had in 2010
- which did not work.
There was more blind hope than skepticism in my mind. Even if
later I find that over time it was a failure,
was it not worth a try?
The alternatives available earlier this year included juggling of
castration methods and chemical blockade of
testosterone, and then inevitable metastasis and a slow death with
one chemical after another. The Internet is
riddled with postings by men who are diagnosed with Pca, then get
treated, and a few find they really do get r
emission but many then go for years living with Pca and suffering
the sexual mutilation and premature ageing
of the treatments. They stop posting about about it. The ones who
continue posting are those battling on, with
some having their wives or children posting when the man has
become quite sick, and facing the inevitable.
Was I not going to go down over time?
I have been sitting on Puff The Magic Prostate Grenade since
diagnosis in 2009, and it is likely to explode
any time soon. The Medical System failed to protect me by ensuring
early diagnosis because the Australian
Psa threshold level for treatment is 5.0. It is 3.0 in UK, and had
it been 3.0 here in Oz, I would have been
diagnosed in 2005.
Despite the lack of evidence held by the top Epworth
professionals, I gave my uninformed consent to proceed.
There was a diligent team of young bright radiation operators at
the Epworth Centre. There was more than one
team, and all were busy, but reliably punctual and friendly.
The estimate of costs was presented to me at $22,000 at July 2. I
had to pay large invoices each week,
without having any clear indication of what the items were or what
the Medicare refund would be. The costs
at end of treatment ballooned to about $26,000, with some
outstanding bills still to be paid when I get some
explanation of what was done when I discuss all the invoices
with a Medicare staff member. So far, Medicare
has paid me about $11,000. The Epworth staff said a private health
insurance fund would not have covered
my costs to any greater extent.
Not all the item numbers listed in invoices at a Private hospitals
will attract a large payment from Medicare.
So when you go to Epworth, make sure you are flush with cash
before you turn up. The sobering thought is
that this treatment in the USA would have cost $50,000, and there
would be no Medicare funding, and the
cost of a 6 week stay in USA would be very high.
I returned to ACT on August 9, and waited a week, then had a Psa
test which measured 0.73, so Psa had
fallen to 1/4 of the level it had been before IMRT.
The doctor said I might see a Psa "flare", ie, a rise of Psa
immediately after IMRT. and then he said Psa
should fall. The Psa did not flare, it just dropped, and then has
continued to drop over last 6 weeks to 0.51
at 21 September.
HOWEVER, I am very skeptical about whether the IMRT achieved any
Pca reduction.
The EBRT in 2010 did little to halt my Pca. ACT doctors told me
the EBRT could work a miracle.
But St Vincent's Hospital In Sydney have a document on their
website which says Gleason 9 tumours like mine
have only 10% chance of being stopped with EBRT. Basically, the
surgeon in ACT who attempted the RP in
2010 found too much cancer to proceed, then palmed me off to the
next best treatment, radiotherapy,
and those guys seemed stupidly optimistic, and offered me nothing
else, which at the time could have been
brachytherapy........
The ADT has been main agent to keep my Psa low.
Before I began the IMRT in mid July, I also began to take 50mg
Cosudex pills each day. Gary Shultz
recommended that the daily dose should be 150mg, but the Epworth
doctor said 50mg was plenty.
So why did they allow me to have a lesser dose than recommended by
Gary Shultz in USA?
I was told by an old lady radiation nurse that 150mg pills were
not available in Australia. I asked if I should
take 3 x 50mg pills a day. There was never a clear answer. More
BULLSHIT. Cosudex acts to block
testosterone getting into receptor cells at the PG tumor. So with
Lucrin to reduce the level of testosterone,
50mg / day may be enough to give enough blockading. How was I to
really know? The idea behind RT is to
damage Pca DNA, and then the lack of available testosterone
prevents cell division and re-growth so Pca cells
are more likely to die instead. Its a good common sense theory,
but the reality of cancer chemistry is far more
complex, and not all known.
But older Pca tumors can grow more testosterone receptor cells in
response to lower amounts of testosterone
due to ADT. Continuing Cosudex just further stimulates receptor
cell production so that no amount of Cosudex
will block all testosterone to cause Pca cell death.
In 2010, I began with a month of Cosudex before injections of
Eligard began. This was said to give less side
effects than starting with Eligard without Cosudex. Probably,
Eligard ( or Lucrin etc ) takes a long time to begin
reducing testosterone, so docs go for the thing that gives a
quickest drop in Psa. They may not have liked to
keep me on Cosudex after starting Eligard because it may have
provoked the tumor to become ADT resistant
earlier than it would otherwise.
I did think continuous Eligard plus Cosudex may have been better
after April 2010, but now think the ADT
failure now seen would have occurred sooner.
ADT does not ever cure Pca, it merely slows it all down for
awhile, in my case, by about 6 years.
Before 2016, the only time I was given Cosudex was at the
beginning of ADT ( Eligard or Lucrin) to
"lessen side effects" of ADT for a month before commencing ADT.
Not a word was said about what
Cosudex actually did. But it has always caused a rapid initial
fall of my Psa, and most of what I am seeing
now is probably due to this chemical.
I missed the monthly shot of Lucrin for July. However these
monthly shots have at least a month of overlap if
you miss an injection.
Whether the IMRT has worked at all will become obvious in years
ahead if Psa continues to fall, and especially
if I have stop the ADT with Lucrin and blockade with Cosudex.
The latest Psa graph update shows a rapid decline of Psa level
between 18 July and 16 August. Between 16
August and 22 September, about 5 weeks, Psa fell from 0.73 to 0.51
in 37days.
Therefore the "Psa halving rate" is now 64 days, about 2 months.
If that trend continues then in 6 months
after 16 August the Psa may be 0.1, in February 2017. If Psa rate
of fall was linear, Psa would be zero
by some time in January 2017. Cancer is a disease that can rise
logarithmically 2,4,8,16,32 because cell
numbers double after a time period. But I doubt the rate of
decline of cancer cells cannot even be predicted,
although some cancers cease their existence abruptly when surgery
succeeds to remove all of it.
I gave up all alcohol in July 2014 and I see NO REASON to break
out champagne to celebrate a win.
So, forecasting future Psa level can be an irrational form of
stupidity. Nobody could ever make any reliable
forecast. In another month my Psa may well begin to rise again
without me having much way to stop it, apart
from chemo therapy, and while taking measures to better manage the
suppression and blockading of
testosterone.
For the first two weeks after my return to ACT after the 5 week
"Medical Holiday", I thought I had escaped
sustaining radiation side effects. But then 2 weeks after
treatment, WHAMMO, I am hit suddenly with severe
diarrhea and my bowel producing large gas and mucus flows and
uncontrollable bowel irregularity.
I've had 2 weeks of fecal incontinence and "explosive shitting
events" where I filled underwear with poo
while rushing to a toilet. The usually good rhythm of bowel has
gone, and my rectum seems badly affected
by radiation.
There are warnings in literature about EBRT. There are side
effects, and I had them all, but not as badly
as some other fellows. Epworth offered protection against side
effects to rectum by the installation of a
hydrogel pad between rectum and PG. I am having much worse bowel
troubles now than I had after the
radiation in 2010 after the EBRT. So was the hydrogel inserted
properly? Methinks the doctor who
inserted 3 RF beacons to my PG and the hydrogel needs to
much improve his methods. I will not say
the word incompetent. It remains to be seen how well I
recover in coming weeks and months.
My condition is now being monitored by my GP and whoever else may
help, and it seems I am suffering
severe acute colitis after radiation. Google is full of
information with videos about this terrible condition
which could go on indefinitely. Just what may possibly be done to
alleviate the effects quite unclear so far,
but I probably will have to be seen by a gastro doc. I am not
bleeding much, but continue with little regularity
some pain, and discharge of gas and mucus.
Stop rolling your eyes, all this may happen to YOU.
The literature supporting Calypso and the use of hydrogel may be
misleading. However, probably the
hydrogel does lessen the side effects to rectum.
If you seek similar treatment to what I just had, assume you will
sustain WORSE side effects than the
doctors indicate may occur. Usually they fob off everything you
say, avoid all difficult questions.
They just want you to accept treatment to keep their income coming
in.
I do not know if the bowel damage sustained at Epworth will be
permanent. There have been cases at
other hospitals around the world where much worse damage to
bowel/rectum has been sustained despite
evidence suggesting that damage would occur.
I read of a classic case in Sweden in 2003 described by caption
"how not to do radiation". They just
repeated normal EBRT like I had in 2010, and over half the
patients endured the problems with fistulas
forming where a rectum wall ruptures and shit exits into perineal
cavity and with bleeding and infection
and pain. Such bowel/rectum damage can only be fixed by removal of
large section of bowel, formation
of a stoma so an external shit bag can be worn. Radiated tissues
in this operation have to be avoided
because once cut, they do not heal and may bleed for days or
weeks. And the article said there was
not much remission of Pca.
Before going to Epworth, I was still having occasional bleeds from
rectum as a result of EBRT in 2010.
These bleeds were bright red arterial blood which occurred if the
shit was lumpy. There was never more
than half a spoonful. The bleed lasted only seconds. In
2013, a specialist gastro doc could not find
where the bleeds were coming from during a colonoscopy in 2013 to
check for bowel cancer.
He had thought I had piles, but none were found. I met a bloke at
Pca support group who went on a
world cruise after EBRT, and he bled cup-fulls of blood. So he
surely had a "bloody holiday", and I guess
it was a voyage of worry for him and his nice supportive missus.
A week after I began IMRT on July 18, I needed to get up at night
to piss up to 7 times. I began to
need to take a nightly Tamsulosin pill aka Flomaxtra to reduce PG
swelling and resulting constriction
of the prostatic urethra, making pissing slow, and laboured.
I continue taking a Flomax pill each night since I began treatment
to get a better sleep. The bladder
seems to have survived. I still can stop or start flow at will.
But experts say that the control I have now
will reduce to complete urine continence because of long term
radiation damage. The radiation doc told
me the May scan indicated my bladder wall muscle has much
thickened because of its extra work over
last 7 years to squeeze the piss through a reduced size of
prostatic urethra. Once my bladder decides to
squeeze, I need to get to a loo fast or the sphincter control is
insufficient while trying to stop the pissing
with pelvic floor muscles. Keeping a piss bottle handy when not
close to a toilet is completely sensible !!
I spend 95% of my time alone, and there is nobody such as a fussy
wife to become upset by seeing an
old man easing a problem in a practical manner.
I have a date with a continence nurse soon to discuss better ways
to manage degradation of my bladder
and bowel function by radiation.
On July 1 I had the gel inserted and 3 RF beacons inserted to PG
tissue using some kind of applicator tool
and guided by ultrasound. The beacon position in the PG is
somewhat critical to ensure the beacons can give
the right information to guide the IMRT Varian machine using
Calypso software. If the PG position moves
during IMRT, the beams follow the moving target - in theory - and
just how successful this is anyone's guess.
The beacon applicator tool was never described to me, but it was a
"transient" procedure, and doc cited
difficulty with the tissue hardness of my PG. I felt I was among
fools who blamed me or their tools for their difficulties.
The beacon implants and gel insert was done between 12noon and
1pm, Friday 1July. Because I was
unaccompanied by a partner or carer, I was compelled to stay a
night at Epworth ( at a cost of $860 I later found ).
I was not permitted to just go back to a hotel room, which
was normal for other Calypso IMRT patients who
were having IMRT following an RP. But it turned out to be
necessary for the night's
stay.
Blockage and inconveniences.
At 8pm, 7 hours after beacon implanting, I could not piss. I dosed
off, and at 2:30AM I remained blocked.
I asked the ward nurse to phone the doctor about what next. The
male nurse spoke poor English and seemed
incompetent and un-communicative, inspiring no confidence in me.
But the phone call occurred, and it worried
the doc who had done the beacon insert.
An intern arrived at bedside with a catheter, another poor English
speaker, and he was very nervous about
what he had to do. I had to calm him down, and prevent over
eagerness to push catheter lest it rupture my
urethra somewhere. We got it done OK, and I have NO APOLOGIES to
anyone for being quite SURLY
about it all when I wasn't trying to calm upset middle aged male
nurses easily offended, and from Philippines
or south America, it seemed. No pretty girl nurses in wards at
3AM, no specialist doctors either.
The catheter was pushed through a soft blood clot which blocked
the prostatic urethra. The bleeding
continued for some hours with blood seeping
backwards up into bladder. I spent a second day at Epworth (
another $860 ) until they were happy for
catheter to be removed and bleeding had subsided enough for me to
be "sent home", ie, to my lodging at
Ryder Cheshire, a place run by a charity entity.
The cause of bleeding was never fully understood by docs. They
admitted nothing. I figured blood from
within cut prostate tissue with beacons had found an exit pathway
via sperm ducts to the prostatic urethra,
where it was able to pool and form a clot and urethra blockage to
stop urine flow from bladder to penile urethra.
The catheter must have pushed through the blood clot, and urine
mixed with blood flowed out immediately.
More blood may have flowed backwards to bladder from bleeding
prostate to bladder and around the
outside of catheter. I did not bleed from penis while catheter was
inserted. These details were not understood
by the doctors.
I did get a visit from the insert doc on morning after blockage
who said he did have difficulties, and that I was
THE FIRST patient to be having salvation radiation after having
had only EBRT as primary treatment.
The removal of catheter was without pain, and I was allowed to
leave to go back to my lodgings at
Cheshire-Ryder Homes on the Sunday after the Friday operation.
During the next 10 days up to July 10 when
I was due to begin RT, I was able to email doctors to question
their methods. During the first week my emails
with doctors indicated they did not know whether they had
punctured my bladder or punctured my prostatic
urethra or both while trying to insert the 3 RF beacons. Without
spelling it out, the doc inserting beacons could
not see what he was doing. The Ultrasound image maker used to
monitor such things was not letting him see
clearly. So he was stabbing in the dark.
On the second morning of my hospital stay, another doc arrived to
chat. He said he had done
,500 brachy-therapies, and he said less than 1 in 60 patients had
bleeding problems and that most of those were
like me, from interstate, and he didn't know why. Nor did I
because such info was just irrelevant bullshit; why was
he there? why talk to me? what magic thing was he going to do to
alleviate my problems? - nothing he could think of.
But, brachy-therapy patients can have up to a hundred radioactive
needle size inserts injected into PG with a
special tool, less than 2mm dia, and all the little needle stick
injuries all heal within a day because they are still
mainly healthy, and heal up before the radiation from inserts
affects them. Brachytherapy can deliver 150Gy to PG,
and with fewer side effects to bowels or rectum, so it has been
the best RT available. But once PG has been given
70Gy from EBRT, or more from BT, then later the PG blood vessels
will not heal quickly if they are cut by any
surgical procedure.
The BT radiation is known as the best type to have. But it is more
expensive, and in 2009, was not available for
me as far as I knew. No doctor mentioned I should get it. Besides,
its only radiation, and with a Gleason 9 tumour,
the chance of it working was only 50% - maybe. I was told to have
EBRT, it was supposed to be as good, but it
just ain't, and later I found St Vincents's Hospital in Sydney has
literature at their website which says the probability
of Pca recurrence after EBRT for a Gleason 9 tumour was 90%.
Brachy therapy BT may have been marginally
more effective than EBRT for my high grade tumour.
I explained to both these visiting docs that success of
interplanetary space missions depended on rocket scientists
having to investigate every possible way shit can happen. I'd been
previously well radiated, and both docs didn't
see that I was probably 100% likely to bleed, and I was not in the
category of the 1.66% of BT patients who
bleed after BT insertions. I suspect the hospital charged me for
the unwarranted unwanted chat on Sunday
morning.
Most docs are not driven by charity, and the Sunday doc must have
been curious, maybe informed by other
doc. And my payments to Epworth paid for his curiosity. The 2 days
in hospital because of bleeding cost
$1,700, with none reimbursed by Medicare.
After being told I was the first patient for re-radiation and this
made me realize I was nothing more than a
laboratory rat for docs to experiment upon without ANY useful info
from the USA doc who recommends
this process. If the docs want my respect, they must earn
it.
I left the Epworth Free Masons ward on Sunday afternoon July 3 and
settled in at lodgings run by Ryder Cheshire
which is an independent entity which has volunteer workers only,
except for one lady who does the books for a
total of about 50 one bedroom apartments with two beds for the
many ppl from faraway regions of Victoria and
NSW. Maybe there were 40 ppl staying, with many cases of breast
and prostate cancers. This WONDERFUL
place allows allows patients and partners or guardians / carers to
have cheap lodgings for a typical stay of 6
weeks. One woman had had 29 courses of radiation, others had lost
a lung, or were in a much worse position
than myself.
THAT was humbling.
I walked a kilometer to shops for basic groceries, and knees felt
very sore, and I was still bleeding from dick
a bit from minor op 2 days before. I had another week to wait
before being "measured up" before another week
of radiation planning. Those first 2 weeks of my stay at Cheshire
was very pleasant, and there was a mobility
scooter available which I used to go to shops, and to a fine
Lebanese restaurant, the Gorgia Cafe in Ivanhoe
which became my daily eatery for the 2 weeks where there was no
daily radiation.
They had Wi-Fi, so I could email the doc to ask so many questions
about why I had bled. I asked what evidence
supported the claims by Dr Gary Shultz in USA. The bleeding kept
going for a week, and I do not know if I bled
from incision entry point for beacons into the perineal area.
During the 2 weeks with no radiation, I asked more questions and
ended up asking the radiation doc to email
Dr Shultz to find out more. He sure was not going to do that. I
said better methods are needed for placing RF
beacons to avoid damaging or cutting things like bladder or
prostatic urethra during injections. I said he will have
other patients like me so he needed to be ready with improved
methods. It is possible he totally ignored all I typed.
He ended up admitting there was no information available about Dr
Shultz's patients and that I had now been
fully informed and that was that. In other words, there was no
supporting evidence that the RT he offered was
much good at all. Hence I had given my uninformed consent. We both
knew it may not work as planned.
10 days after the minor surgery, I did try to visit an aquatic
center near my lodgings to swim a bit, 400M, and
I bled again, so I gave up all silly notions of doing any exercise
while in Melbourne.
The radiation treatments began on 18 July and were completed on
August 9. At 10AM each day I had IMRT
to PG and to upper chest targets. At 4PM I had a second round of
IMRT to PG only. I filled in time by doing
web-page work with my laptop. There were 4 radiation staff and 2
nurses in an office who had little to do
with me except to lecture me about having a gas free and shit free
rectum. They managed to give me enough
potty training to always arrive gas&shit free for RT, and with
500ml of water in bladder. After return to ACT,
I have had 3 brief emails from the head radiation doc asking about
my bladder and bowels. All was cordial
without me bashing the man with questions was never going to
answer. He must have winced when he tried to
read the screen fulls of history and suggestions and about my
terrible fecal incontinence. I doubt he read much
at all. I am not officially in his care any longer, and there's
little need to contact him. He may read this here.
A week after I returned to ACT, I climbed back onto bicycle. No
more bleeding. The entry point for surgical
gadgets under crutch had healed OK - not radiated. I was able to
increase distance and speed, and I regained
my fitness levels close to what I had in mid July before the
Melbourne trip. But I did notice that I breathed more
heavily riding uphill, and there has been some damage to lung
tissue. The doc did say I might have some difficulty
swallowing and a sore esophagus, but I had neither. I seemed to
burp more and suffer some slight indigestion.
Appetite has remained good but since August 9, and increased bowel
irregularity has not stopped me eating the
same vegetarian diet. However, I like to make my salads with green
fresh green vegetables which i can heat in
microwave to make them more easily digested. There is no need for
so much raw food.
Weight has bounced down a Kg while in Melbourne, then up 2Kg, then
down again, as irregularity manifests itself
with erratic disposal of bowel biomass. Once past the acute
irregular shit-in-pants events, I now have a regular
form of irregularity, with rectum not happy with handling shit,
and wanting to spurt mucus and gas at least 10 times
a day.
My resting heart rate in mornings is 50, up slightly from the 48
last July. it takes more time for HR to go lower
even after short rides. I have a pain in the lung on right side,
similar to having cracked rib some years ago, so
I assume I have poorer lung function, so heart beats faster to get
more blood around to be oxygenated at the
lower rate. So the Melbourne treatment had a slight worsening
effect on my cardio vascular health. I was told the
two distant Pca spots were in 2 lymph nodes. Their position looked
like they were in my lungs. I have ZERO idea
of exactly what was radiated in upper thorax; the machine is able
to gain enough info from scans to aim at whatever
volumes are on scan without any other tests able to proove that
indeed the spots were at lymph nodes, and not
within my lungs. So I can only cross my fingers. I am just a dumb
( and irritating patient ) who just cannot trust
the education and experience of doctors unless they proove they
know what they are doing. The world is full of
well educated fools on good wages, and beyond anyone's ability to
scrutinize their efforts. Shakespeare wrote
many plays about powerful blokes and sheilas who were were so
flawed......
Last February, I joined the the waiting list for two new knee
joints at Calvary Hospital in Canberra.
Walking further than 100M has become painful, and scans in 2014
proved I need two new joints, all propelled
by the crummy genetics I inherited from my dearest mother's genes.
She hated all vigorous exercise, and I never
ever saw her raise a sweat. She did like to swim, and I watched
her extremely slow motion in a pool where I
took her when she was 73. She got through to 98 years of life as a
mindful plodder, an attribute we both had.
She had few athletic attributes which allowed others to do twice
what she did. I am much the same, but I
inherited my father's zest for exercise; he set a schoolboy record
for The Mile in about 1924, and rowed
well for the posh school. He was always ready for real stinky
sweaty work for real men and I often helped
him eagerly with the work around the house and at his vet
practice. But he neglected a melanoma on his leg,
and he died at 60.
If my cancer continues to outwit the doctors and I need chemo
therapy, I won't get those new knees.
The waiting list was 12 months, but Calvary contacted me for
pre-admission in mid August. I told them I
needed more time to allow doctors to decide if I was likely to
have a long remission time and hence allow the
knee surgery. It would be extremely pleasant to be able to walk
800meters to the local shop and, and that would
greatly help my health and help reduce bone density loss due not
using legs walking. I could also ride a lot further,
and I can say I would be most eager to do all the rehabilitation
needed after knee surgery.
During time in Melbourne, for weekdays with radiation there were
cars provided to get patients from Ryder
Cheshire to several hospitals, all driven by eager volunteers
between 55 and 70. Ryder Cheshire is about
10km away from hospitals in Richmond. The private hospitals'
policies give local transport to the sick coming
from all around Victoria and NSW. It helps make the big services
of big hospitals available to those in remote
regions without the stress of getting around in a big city.
There were some spirited discussions every other day
on the 1/2 hour drives from "home" to the hospitals. Most patients
had only one radiation session per day, so they
were driven home by the volunteers before lunch. I was the only
one getting two radiations per day, at least 6 hours
apart, and Epworth Centre staff gave me taxi vouchers for a free
ride home in slow peak hour traffic which cost
an average of $33. It meant I did not have to walk in pain on bad
knees. For those who can walk, there is also a
good train service from Ivanhoe to West Richmond station, 300
meters from the Epworth center. From a station
at Ivanhoe, bus 548, which reduces 1.4km walk from station to
Ryder Cheshire to 300M. There are also taxis
from station to Ryder. I may have had to stand while using public
at peak hour times. Epworth did not charge
me for vouches worth a total of about $660. They still probably
made a healthy profit from the total of
$26,000 they charged me. I would not be surprised.
Ryder Cheshire refused to take a cent from me for the
accommodation. They didn't seem to know what rate to
charge me, which depended on whether Epworth would pay them, at a
higher rate than they felt they could charge
me if I paid direct, ie, $20 per night for 31 nights. I suspect
Epworth did pay them, and paid $38 per night, and
the Epworth accounts had no item for accommodations. I have no
idea who paid who, but probably the
accommodation costs are buried in the invoices from Epworth. I
filled out forms to claim for ACT Government
assisted travel expenses. I never heard a word from ACT Govt, for
this little used service. The accounting of
costs at Epworth seemed unclear, but Medicare staff in Canberra
said all was well with their charges.
I gave the Ryder Cheshire a donation of $1,000 before I left. If
I'd had to pay for a Hotel at $100 per night,
If have paid $3,100, and not had access to the daily transport to
hospitals, and not had a tiny bedsitter flat to
cook in, my costs would have been far higher. If I ever need to
get medical treatment in Melbourne again, I'd
want to stay at Cheshire Ryder. It is a lovely simple old
fashioned place to stay with ppl about who have troubles
like me.
-------------------------------------------------------------------------------------------------------------------
Before my Melbourne treatments a gentleman emailed me to to
describe his IMRT which followed his RP
some months before at Epworth Hospital to which I went. I'd met
Paul online in 2004 I gave him details for a
component he wanted to make for an audio amp he was making. We
still share an interest in DIY Hi-Fi
technologies. His descriptions of what happened to him gave me
confidence that side effects for IMRT
might be minimal, and that radiation treatment itself was quite
tolerable, and that the hospital staff were very
nice. Most of this turned out to be quite true.
After his RP, his Psa went very low, then began to rise. He then
had the surgery site radiated using Calypso
IMRT, and Psa went down again. I met him in Melbourne and had
dinner with him twice.
But some months later, his Psa is rising again, showing that Pca
is progressing despite all the surgery and RT.
Because his Psa went so low after the treatments, it was unlikely
there were metastases somewhere.
When Psa does not decrease much, it could mean there is Psa coming
from a metastasis.
I'd say he will have to go to ADT, and probably he may suppress
his Pca for some years like me, until the
Pca becomes castration resistant which is usually inevitable.
I began with PG that was NOT removed because the doctor said I had
an inoperable Gleason 9 tumour
which had slightly escaped the PG capsule- a monster. Paul will
live many years yet, and probably more
years than I will, and I'm 10 years older, and much more likely to
go down in 5 years, before any magic
cure arrives.
Good links...
Subscribe to this site for continual emails of latest progress in
research and drug trials :-
https://prostatecancerinfolink.net
Psa level between age 40 and 60 indicate lethal Pca in later years
:-
https://prostatecancerinfolink.net/2016/06/14/another-step-toward-a-rational-risk-stratified-psa-testing-methodology/
If Psa is above 1.0 at age 59 there is good reason to worry.......
Reading:-
http://www.prostateoncology.com/education/glossary/a:hormonal_therapy
http://prostatecanceruk.org/for-health-professionals/latest-research
------------------------------------------------------------------------------------------------------------------
Before 29 May 2016.
My prostate cancer progress presents a bigger battle in coming
months. All those people who said I would
get better and that I didn't have anything to worry about and that
alternative therapies would work WERE
ALL WRONG. Today I cycled 45km to give a total of 136km for the
last week.
Weight is 84.2Kg, resting heart rate = 52 bpm at 1 hour after the
ride, 48 bpm this AM, and nice steady
beats with no double beats or missed beats. My vegans diet is
continuing, and I have to be honest, its 95%
vegans because I do allow low fat milk for my tea, and 150 grams
of salmon from fish farms in Tasmania.
I quit all coffee 2 months ago after realizing it contributed to
feeling too hyper after 3 coffees, and probably
caused a bout of uneven fast and slow HR just after last X-mas.
I've been on ADT aka HT to block my
testosterone production since 2010, so 6 years now, and I had an
eight month pause in 2012-2013, and a
gain last year 2015 for 5 months. After both pauses the Psa shot
back up. Since the last pause and after
recommencing HT last August 2015, Psa went to a low of 1.0, and
then began to rise to 1.5 by April 2016.
Its now 2.3 so it is doubling each 4 months, fast, and HT with
Lucrin injections is not able to keep testosterone
below 0.5 for adequate suppression of testosterone, hence Psa is
rising, and Psa would be 128 in 2 years if
nothing is done about the situation.Before 4 May 2016 I could not
find any available trials of new treatments
in Australia.
But when I last spoke with my good oncologist he suggested I go to
a Melbourne imaging clinic and consult
with a Melbourne radiologist at Epworth Hospital. These together
offered the new benefit of an MPSA +PET
scan which shows my cancer status and is a guide to choice of
further beam radiation using the Calypso IMRT
method :-
http://www.wesleymedicalimaging.com.au/uploads/file/New%20PET%20Studies/PSMA.pdf
Calypso seems to be the best way to deliver RT to prostate tumors
with much less damage to surrounding
organs or bones. I had previous EBRT in 2010 with probable
radiation levels of 65Gy, with some side effects
on bowels. The proposed Calypso IMRT uses computer program and
implanted RF beacons and hydrogel to
much reduce side effects to bladder and bowel.
There are online articles on Calypso such as.
...
http://www.sciencedirect.com/science/article/pii/S0360301606032767
There are plenty more, and these may confuse patients and make
them anxious unless you are a naturally
scientifically minded person like myself.
I also found a video suggesting IMRT was no better than older
EBRT,
https://www.youtube.com/watch?v=XWobSwAnP68
But I think the IMRT is a much better way to deliver RT for me.
Doctors like to tell us to stay away from
Internet which makes us anxious and confused, and just rely on
their learning and experience. But much of
what many doctors told me made me anxious and confused.
The anxiety and confusion did not last long in my mind because
usually what the doctor says agrees with
what I find on the Internet, and I have a rational mind. Many
modern clinical treatments have been
developed over many years of trials which have been regulated by
government organizations.
But regulated systems don't always keep patients safe. For
example, I should have had a biopsy when
Psa reached 3.0, some years before my Psa climbed to 5.0 when the
Gleason score had increased to
dangerous 9 and Pca tumour was inoperable !
But the fact remains that modern medicine does more good than
harm, and I would be dead now without
the treatment I have had.But despite all the modern wonders of
treatment, prostate cancer manages to kill
33% of men diagnosed. It is highly likely to kill me because I was
diagnosed too late, even after having
regular Psa tests, and then finding I had a Gleason 9 tumour with
aggressive cell type.
The doctor at Epworth Hospital is the first doctor who was happy
to email me with with considerable
information. The IMRT he proposes does seem safe to me, it means
31.2Gy are to be applied in 26
sessions over 3 weeks, which in theory raises total radiation for
my PG to 96.2Grey. The doctor
supplied a paper published in American Journal of Clinical
Medicine, Fall, 2011, Page 170, where
one Dr Gary Shultz claims he gave repeated RT to 45 men who ALL
had a positive outcome, ie,
Psa began to fall.
http://www.aapsus.org/wp-content/uploads/ajcmeleven.pdf
I am seeing my good oncologist on 31 May, and my urologist on 8
June, and I will also see the
radiologist who did my EBRT in 2010, on maybe 14 June,
to discuss the following :-
1. Details of small amount of Pca spread to 2 lymph nodes in upper
thorax.
2. Permissible maximum amount of accumulated radiation to PG.
3. Case histories of patients with similar Pca progress who have
had two repeated courses of RT.
4. Possible side effects of bleeding from blood vessels of PG,
5. Possible dysfunction of prostatic urethra, including
disintegration, or stricture, interfering with urination.
6. Possible alternative surgery involving removal of bladder, PG
and formation of stoma to allow ureters
from kidneys to drain urine to external plastic bag. ( 40,000 ppl
in Oz wear bags for body waste due to
cancer or road crashes et all, and they have a good life. )
7. Whatever else they tell me, or what I forgot to include here.
I learnt much from Internet from research hospital publications
online, Sloan Kettering et all.
Doctors have yet to get rid of my prostate cancer, and quite a
number of treatment plans did not
work despite their best intentions and predictions, and to me, not
reading the Internet would be
like poking my head in the sand. Am I not entitled to get my info
from the Internet just like doctors?
The new PsMa scans have become available in last 12 months, and
are on trial in Oz.
It seems the supply of patients for a trial are supplied by a
referring doctor, so I probably had no
chance of getting into any trial without a doctor's referral.
My local Canberra oncologist and radiologist both said they had
referred patients like me to hospitals
in bigger cities such as Sydney of Melbourne where a bigger range
of specialist services and treatments
are slowly becoming available. My local oncologist said patients
he sent away to Melbourne were
helped, but not exactly how many or how their life improved, so I
am yet again left to assume there
may be some increased lifetime and there was no talk of a cure or
remission.
I am sitting on my Prostate Grenade, and while its growth
activities have been slowed by HT, it does
not mean it will just die and fade away. It will slowly swell up
and try to choke my prostatic urethra
which will slow my flow to a dribble and affect my kidneys. If
left alone, it will evolve to become a
worse form of cancer which is more likely to spread in a rush -
the grenade pin falls out, and floods
my blood stream with Pca, and overwhelms my immune system.
The proposed IMRT is the Last Chance
I have to intervene with available treatment in Australia afaik.
If this treatment fails, then I will have to
begin chemotherapy, not something anyone can look forward to.
The expense is minimal for the PET scans and course of radiation,
and there are costs for travel
and accommodation. Not much of all this is funded by Medicare.
For 2 days in Melbourne to undergo scans and re-diagnosis, return
air fare was $432 aud with
Virgin, a small room at a Quest hotel was at $150 a night. On
return, I found cheaper accommodation
for $80, which I may use in future. Some of the costs of
travelling outside ACT for medical treatments
may be paid by ACT Govt. There is a special claim form, not much
publicized, and without mention
of funds for air fares.
On Monday 2 May, I had a CT scan with radioactive iodine.
Then I was injected with special solution which is able to bind
Gallium 68 isotope to places where
any Psa is being produced. A PET scanner used to produce the PsMa
scan which tells doctors and
myself just where Psa is being produced now, something nobody has
known since 2010. The scan
is said to be far more sensitive than a CT scan and very low
amounts of Pca are seen. The main
source of Psa is the primary tumour at PG.
On Tuesday 3 May, the radiologist said the PET showed no Pca in
bones, bladder or bowel, rectum,
but there were two small amounts in two upper thorax lymph nodes.
He said these would not be a
major problem and would be fixed after the main primary tumour has
been radiated. I will need to
examine the follow up carefully. Before being sent to Melbourne I
didn't think any more radiation
could be used, but it seems I was incorrect. The Melbourne doc
said it could be at a higher dose than
the original in 2010. Just what that means wasn't clear, was the
total accumulated radiation to be higher?
By how much? My research on Calypso tells me IMRT with 81Gray
levels are possible, above the
probable 65Gy levels of 2010. So was the total radiation level to
be increased to 146Gy? I searched
all over the net to find what was the maximum safe level of
radiation by X-rays for the prostate
gland. Many other parts of body were given nominal maximums, but
not the PG. I assumed 81Gy.
The doc sent me the .pdf showing recommended treatment by Dr Gary
Shultz.
It tells us the IMRT applies 31.2Gray to PG, and when added to say
65Gy with the normal EBRT
the total = 96.2Gy. The EBRT in 2010 wasn't a high enough level to
halt the tumor growth, but must
have caused some damage, and there has been some recovery,
or healing, so the 31.2Gy now
proposed may be well tolerated by healthy tissue, but maybe not
tolerated by Pca.
It is assumed healthy tissue will always survive radiation better
than cancer cells. The cancer growth
depends on a good blood supply which it extends for itself to do
well. Methinks some cancer is could
be much more robust than healthy tissue, and unless all blood
vessels are destroyed by radiation, and
surrounding healthy tissue as well, maybe then the cancer might
just give up.
Any simplistic explanation of how radiation or chemo actually
works is likely to be BULLSHIT.
The original EBRT I had in 2010 used old machines with beams at
only 4 directions, each session
gave 1 shot vertically up, 1 shot vertically down, and 1 shot
horizontal left, 1 shot horizontally right,
with no regard for where the entry and exist beams went, and with
poor dynamic control of beam direction
relative to prostate, and unknown beam shaping to conform with
shape of PG seen in accompanying CT
scanning. PG can vary up to +/- 6mm due to breathing, and bowel
content movements. Therefore beams
are allowed a 10mm margin exceeding the shape of PG, and this
means the rectum walls cop a large
dose of RT. I was expected to drink plenty water before each
session to stretch bladder to keep more
of it away from PG.
The Calypso method allows calculation of the best beam directions
at many angles all worked out on
a computer prior to the radiation. The intensity of radiation is
variable and beam direction is locked on to
tracking information from implanted RF beacons within the PG.
Hydrogel is inserted between PG and
rectum and I assume bladder as well to nudge these adjacent organs
12mm away from PG, So the beam
control uses a much more sophisticated computer control program, a
benefit of progress over last 20 years,
and thus offers less side effects, and raises the amount of RT
allowed to be given to PG. The hydrogel
hardens to being like rubber immediately after insertion, but
dissolves away during 4 following months.
Its is said to be entirely inert, and safe to use.
I don't expect very much additional radiation damage to what I
have had already, except to prostatic
urethra, all nerves, and thus may bring incontinence.
The doc said the IMRT can be over a week, or 3 weeks. The week of
RT suits those wanting the
cheaper cost, and shorter accommodation, and less time off work.
Being retired, the longer 3 week
time suits me, and doc said the longer time gave slightly better
results. He said there is a chance
the Tumor Cells Will Be Exterminated. A bit like a Darlek in a Dr
Who episode.
Well OK, sure, but all exterminated? will some just modify
themselves into something worse?
It is cancer we face, and it is real good at making a fool out of
many doctors.
A Psa test 6 weeks later would tell me and my doctors who are all
interested if the IMRT has done
anything. Psa is supposed to decline. The worst outcome would be a
rapid rise in Psa. I'll remain on HT,
maybe monthly Lucrin shots, and Cosadex.
I have provisionally agreed to go ahead. The doc in Melbourne is
happy to do the RT if my other
doctors have faith in what is to be done, and of course to get to
see all the doctors I had to book
appointments and get around the waiting times of up to a month
before my turn was available.
There are hundreds of other patients, some in greater need than
me. And I have to wait for one doc
to return from time off, and oncologist takes a break a week after
I see him. So unless you get busy
to talk to these docs, then expect almost no co-ordination or
concern about yourself.
Just make sure you are polite, not ever surly, doctors and
specialists are not God, they are just men
or women, and you must make do with whoever is around and I
believe this approach leads to the best
evidence based treatment you could have. The oncologist didn't
know what Calypso IMRT was about
when I mentioned it. After dealings with me he will learn just
what is on offer; I very much like talking
to my doctors, and I try to bring then a concise list of my
concerns.
Because there is some Pca spread to lymph glands I will have
chemotherapy at a later date, maybe
in 2 months time. Nobody knows what might work, or what
combination of chemicals might work.
Many chemicals merely delay the the end game a few months, but in
some cases it gives years of life.
There are chemo drugs such as abiraterone, enzalutimide, taxotere,
cabazitaxel, etc.One solution might
be the to removal of bladder, PG, and sealing off penile urethra.
Then the two ureters from each kidney
are brought together to make a join to a hole at side of lower
abdomen for external urine bag.
But because my Pca has some slight systemic spread the surgeon may
feel it is a pointless exercise.
I know a guy who has been through this, he's lived happily onwards
after this op and gets jobs done
around the house and his wife still loves him.
Many websites are a cause of confusion and anxiety, but I found
this from the UK...
http://www.cuh.org.uk/bladder-cancer/your-stories/alan-hoensch
The PET scan showed my bladder is not happy. The bladder is
muscular bag with walls normally
3mm thick to expel urine with an easy squeeze to get urine out
along well sized tubing with few restrictions.
But in my case, the urethra in PG is being strangled making it
harder to expel, so the bladder has built up its
muscle thickness to 10mm. I don't realize the effort it makes and
nothing is painful, unless I delay getting to a
loo.
I told the Melbourne doctor that men should be able to have their
PG removed before cancer spoils their
fun, and before cancer makes it impossible to spare nerves. But he
said no 25yo would want this, but I
said many over 55 would much like it, and they are usually able to
afford it. It is rich old men who fund old
men's cancer research and treatments.
But prostate surgery often leaves a small number of Pca cells
behind, or healthy PG cells which will develop
Pca later if the DNA allows it. I know about 5 men my age well
enough to know their Pg condition; all had
surgery, and all had Pca return, and all had "salvation treatment"
with RT. Some had HT, while others didn't,
so the HT was a spare weapon up their sleeve if the Pca
progressed.
One friend had surgery over 6 yrs ago, Psa went down to < 0.02
after a year, then hovered for a year or two,
then began to rise to 0.7 before last December. He then had 35
sessions of EBRT over a month to the area
where bladder was joined to urethra. His Psa is now 0.1, and
apparently falling. But his tumour was Gleason 6,
and the target for RT was small, so "salvation" RT is more likely
to work. I had Gleason 9, aggressive cells,
operation was impossible and I'm in a much worse situation.
There are idiots who suggest Psa testing is all BS, and treatment
does not extend life very much.
But I would now be dead if Psa tests and treatments had not been
available.
While surfing the Internet I just found a .pdf document prepared
by St Vincents Clinic in Sydney about
the range of things done at this clinic.
https://stvincentsclinic.com.au/wps/wcm/connect/d4f26437-5af8-46b6-bbed-981b66d7616e/2014+Proceedings.pdf?MOD=AJPERES&CONVERT_TO=url&CACHEID=d4f26437-5af8-46b6-bbed-981b66d7616e
On page 11, there is a table giving Psa levels at which referral
to a urologist should occur.
For men of 60-69, the Psa level is 3.0. My Psa would have exceeded
3.0 well before 60, and my
GP did not send me to a urologist until Psa went close to 5.0 in
2009, when the tumour had grown to be
inoperable and with aggressive cells.
So I cannot stress how important it is to be diagnosed early,
which means a biopsy at Psa = 3.0, regardless
of other public health guidelines based on Psa of 5.0.
Other good reading about radiotherapy, UK
http://www.cancerresearchuk.org/about-cancer/type/prostate-cancer/treatment/radiotherapy/external-radiotherapy-for-prostate-cancer
General info about survival rates, USA
http://www.harvardprostateknowledge.org/how-to-handle-a-relapse-after-treatment-for-prostate-cancer
From what the Harvard site says, I had a 90% chance of recurrence
of Pca after the "normal" level of EBRT
used at Canberra Hospital. The recurrence of Pca was masked by
action of HT, so the recurrence was seen
in three rises of Psa when I ceased HT 18 months after initial RT.
The maximum rate of Psa rise was much faster
than 2ng/L per year.
-------------------------------------------------------------------------------------------
My vegans diet includes large amounts of raw vegetables and herbs
in salads, and regular quinoa plus
almonds boiled together, tiny amounts of low fat milk, sugar,
salt. I use virgin olive oil in many things, but it
amounts to less than everyone else's fat intake. I don't eat any
junk food, ever, no chips, deep fried anything,
no alcohol, no coffee, no cheese, and I really don't know anyone
else who eats like I do. The ONLY way
ppl get fat is because they eat too much. Regardless of all other
considerations or invented feel-good
justifications or theories anyone anywhere says about food and
weight, if you stack on more weight beyond
what is ideal for you at 35, ie, when your BMI should have been
less than 25, then you have eaten too much.
I was at my fittest at 42, and weighed 82Kg. I could ride a
bicycle 300km in a day at 28kph average. And I
have quite poor athletic genes. I'm now 84Kg, and bike speed is
now down to 20kph because muscles have
weakened at 69, and I've been chemically castrated for 6 years
now. The weight change is about -5Kg muscle,
+7Kg fat, but I still have BMI about 25.0. Despite the terrible
condition of my knees which need titanium joints,
I still manage to ride over 100km a week.
I weigh myself naked each morning on electronic scales, and plot
each day's starting weight on a graph in my
hand-written journal I've been doing for last 55 years. Only one
person controls food flow down your neck,
HE IS YOU.
What you eat should be full of vitamins and micro-nutrients. As we
age, we need less food calories, but we
need good nutrition. We have less muscle weight and we do not need
extra protein or extra carbohydrates;
you need less of all things which are calorific.
Breakfast for me is a bowl of chopped raw kale, one raw tomato,
one spoon of olive oil, a sprinkle of turmeric
and salt with iodine, and a pot of green tea. I don't need to eat
between 8am and midday. Lunch is one
vegetable only sandwich and a pot of tea. I found it very easy to
accept the more frugal existence despite
my improved finances and the booming roar of advertising shouting
at me to eat and drink garbage, and
spend my way to being happy.
Over eating is poisonous, over spending makes you sad. Dinner is a
salad with many green things and red
capsicums etc, and staple food is boiled quinoa with some almonds,
which need to be cooked to allow their
goodies to be absorbed. I eat maybe 5 small green apples after
dinner to midnight. Being chemically
castrated means I have almost no testosterone which slows down my
metabolism which has me feeling the
cold more. I am unable to burn excess calories and any slight
excess calories become fat shortly after eating.
-------------------------------------------------------------------------------------
For the first 4 years of ADT, erections rarely ever occurred
spontaneously, but any seductive images if females
brought Roger to life and then this all changed to less often, and
signals to Roger became muddled and only
due to a full bladder unlike previous years where this rarely
happened before treatments.The ADT ruined all
my sexual abilities by end of 2014. Whatever pleasurable
sensations I could have become so dulled that any
possible
sexual excitement became not worth pursuing, and absence of
testosterone has caused penile atrophy, with
fibroids forming in tissues resulting in erectile deformity, ie, a
dick with bend, and very fragile skin. I have the
kind of dick no female would ever want have anything to do with.
Medical treatment for prostate cancer always
kills Roger.
Most men would not prefer to know the results of long term ADT. I
was highly hetero sexual and capable
of pleasing myself or any female until about 2013, 66yo. I have
now accepted that between now and my death
it is highly unlikely any female would ever want to have anything
to do with me at all. Sex with any F after a
certain age becomes a liability - not enjoyable if the F is likely
to be irrationally angry in your face after a few
months, or a few hours. Although I keep thinking about sex, and
having some female company in my life, it is
just my silly dreaming.
Some men would have a penile prosthesis installed, maybe for
$25,000, but in my case I've been radiated and
surgery anywhere in pelvic region is extremely risky because I
could bleed to death due to damaged blood
vessels.
I have not heard of any man able to describe sex favourably in
terms of how he feels during use of a prosthesis.
He would probably be OK if he had RP surgery only and had full
testosterone, and then it should work well.
But if a man has had ADT for over 4 years, his WHOLE sexuality is
buggered. It is normal that with prolonged
testosterone starvation the Roger gets fibroids in the erection
tissues, maximum erect length will decrease from
140mm to 100mm, and it is very likely to have a bend in one
direction, often downwards, so Roger resembles
a brass garden tap. it looks ugly, and penetration would be
difficult to maintain, and the feelings of pleasure all
vanish. The skin around the head of Roger become thin and fragile
where it joins the shaft, and a gentle rub
during a jerk off will easily tear the skin which then takes days
to heal. Erections occur with a full bladder
while asleep, and then a man wakes up, and the erection vanishes
after a pee. Even with an erection brought
on by a Little Blue Pill, and In the presence of a young fully
functional female, a man is not going to do much
good, and the female is likely to flee to a man 30 years younger.
Who could blame her?
The intensity of orgasm declines to zero, and no matter how well
the female performs fellatio, it just becomes
a boring waste of time. So use of a vibrator may do a better job
on the female, but psychologically, it is bullshit,
the young female can only be satisfied by a real man. There
would of course where the female has huge medical
limitations, and is happy that ANY man is able to be
vibrantly intimate with her; but this is actually very rare.
Usually man of 60 has not got to worry about sex with a wife if
she's close to his age. The decline in a woman's
sexuality is dramatic after about 45, and women become frail, they
cannot and will not try to stay fit, and
sometimes they become emotionally erratic and difficult to love,
let alone make love to.
Welcome to the land of Old Age.
Between 2009 when I was diagnosed and 2016, I rode about 90,000 on
a bicycle, and I think I scared away
any possible partners I may have seen. Few women near my age rode
bicycles, and were seriously dismayed
I was in much better health than they were. But then, I had a wife
who left me at age 22, and she
was similarly afflicted by my vibrancy and indestructability. I
was a man they could not root, shoot, or electrocute.
Good, afaiac. Why would I ever let myself be so physically
mediocre and so many others????
I have often thought of marrying my bicycle. It may become
possible in these days of liberation where even
gays can marry. A man could marry his dog maybe. But marrying a
bicycle looks good to me, and why?
Because the man can go for a fukken ride any old time he fukken
wants to!!!.
No back chat, low costs, feels good, and its freedom, and I am
sure the bike loves it too.
Unfortunately, my preaching is to a mass of men who insist that
they destroy themselves by 50 with
becoming unfit and overweight, usually from eating
too much junk food laced with fructose and sucrose, sugar, and too
much alcohol. Their whole life is
one of TOO MUCH.
I found all young women soon vamoosed when the reality of the
required co-operation together caused
a Female Allergic Reaction. Love is such a dreadful threat to so
many ppl. I doubt any doctor has any
answer to the not so uncommon malady of where people look me in
the eye to tell me "I Hate Love".
I once read this written in large painted letters on one of
Canberra's cycle paths. I had a female boarder
in my house for 10 years who one day blurted out "I hate love".
She was a fine responsible tenant to have,
but had zero ability to relate to anyone beyond the non personal.
The fact remains that many ppl hate love. I am often lonely, but
then relieved I am not married to a
Female Dragon who finds fault in all I do, and is like a millstone
around my neck. I gave all women
only ONE CHOICE, to love, and sure, they did for awhile, but then
that stops, and they could not stay,
and they repeated the bullshit on the next male victim. I was
always gentle and understanding when
they departed, while wishing to leave a boot-mark on their arse on
the way out the door. I was far to
polite to all I met.
--------------------------------------------------------------------------------------------------------
17 February 2016
Not much to report since last January. I ceased riding my bike
late last October, and now I am trying
to lose the Kg I put on. Becoming Totally Vegans might do it, and
help prevent the severe effects of
inflammation in my knees. There is theory lurking in minds of
"healthologists" that eating or any other
animal product, eggs, all dairy junk, and cheese junk triggers the
immune response to attack cartilage
because of molecular similarity.
While young, most of us can eat anything without any worry, except
for fact most ppl eat way too much
of everything, and including excess sugar, fats and processed
carbohydrates. But as age embraces us, it
makes us ache in our joints, and the less we do to encourage this,
the better. I find this true for myself and
without knowing if any of a myriad number of theories about diet
and health are in any way true, or proven.
Anyway, for me, a fairly strict vegetarian diet is better than
taking any pain killers, and it is natural to me
to NEVER EVER buy ANY JUNK FOOD, including all meat. Not even
Lindt chocolate bars or a
monthly bottle of red wine. Sure they taste nice, but the health
benefits are extremely low, and whatever
chocolate you eat, you can't avoid the huge fat/sugar content even
though the packaging claims "85% pure
cocoa. With wine at 12.5% alcohol, its much more calorie riddled
than green tea. Anyway, I have slowly
gained a Kg over 3 months, and I thought 150grams of skinless
chicken 3 times a week was OK, but no,
it ain't.
I used to ride for 10 hours a week, and had a need for protein,
but with being sedentary, there's just no
need for so much, and I figured I was getting enough protein for
reduced activity. With chemical castration
with Lucrin, to combat Pca, my body has become unable to burn of
any excess calories. Right now, height
= 1.845M, weight 85Kg, BMI = 24.9 I should be less. Waist is
100cm.
I was 1.865M, and weighed 83Kg, BMI 23.8 when I was very fit and
raced on bicycles in 1980s-90s.
My waist now measures 100cm, and in 1990 it was 90cm or less, and
I had maybe 4Kg less fat and 4Kg
more muscle. Even though my BMI was 24 at 42 , I still had a much
higher fat % than the quickest people
I raced against. I was always at a big disadvantage on hills, and
in time trials the slim guys have less volume
so they cut through the air faster than I could. Naturally,
athletic clubs attract people who are naturally
good at sports, and they beat all the slow coaches like me. Their
ego gets the big lift with wins over those
less endowed with great genes. It was sickening to witness the
constant focus on a win. But occasionally
I did very well in handicap races.
The idea of BMI and waist measurement does not tell us all about a
person. A short weightlifter may have
waist above 100cm, and BMI 30. Weightlifting may be all he can do,
but he can find a happy path in life
like everyone else. We are not all the same. Now as we age, we
reduce muscle weight even if we keep
exercising. About 80% of us get heavier, and lost muscle is
replaced by fat, and BMI can remain the same.
So the weight of muscles I had are replaced by fat, especially
around the gut. There's much more to grab
hold of compared to being 40. We should get LIGHTER as we age, we
all like to live well, and enjoy activity,
like cycling, even though av speed goes down. I have found it is
impossible to get lighter, and I'm 3Kg heavier
than I was when fittest at age 40, so my fat % has probably
doubled.
But at least I don't weigh 100Kg like so many other guys my age.
My limiting factor is now my joints, with knees leading Nature's
charge to reduce my lifestyle. And while
my knees ache, so do hands and wrists and back; whatever my body
is doing, it is having challenges at more
than one place. But after doing anything physical, despite the
aches and pains, I am glad I did it, and my
mind and body both feel better.
Just after last update, about a month ago, I had a bout of heart
fibrillation where HR suddenly went to 120,
and irregular, so I drove to Calvary Hospital where they kept me
there till 1AM. The docs put me on Sotacor,
to slow HR. Within 6 weeks HR went back to normal, and I've now
stopped taking the drug. But I am taking
100mg of Cartia, (aspirin ) daily, if I remember, which may be
thinning blood slightly to lessen the hypo-tension I
suffer. Hypo-tension is not to be confused with hypertension.
Subsequent heart clinic on 16th Feb looked at
heart with Ultrasound, and doc said my heart looked just great. I
said "Hmm, shame about the Pca, I'll be a
good lookin' corpse on the slab after it kills me".
Two weeks ago I had a mechanic fix the brakes on my 1986 Ford
Laser. He had it for 5 days, because
suitable parts were not immediately available. This forced me back
onto bicycle, and I rode 100km last week,
with 15km ride up the hill to the heart clinic. I figured I'd make
it, and all went fine, if I died on the way, so be it.
Doc was not alarmed, but more confident I'd be OK. A bloke of 30
overtook me up steepest hill and maybe he
was trying, but then I caught and passed him just before the
crest. Heck, I'd given the yung turk a 38year
advantage, so I realized I wasn't near death just yet. Don't ask
me what caused the bout of HR bothers, but I
suspect it was eating a few dark red carrots; I'd heard dark red
vegies are very high in a very good anti oxidant.
Maybe too good. I can't be sure. I've only ever had it once before
in 2004, after coming off VIOXX which later
got banned because it killed ppl with heart problems.
Knees didn't ache later as a result of the rides, like they did
back in October. Not as bad as in 2004.
We need to keep exercising.
January 7, 2016. Prostate cancer report.
My last Psa test was 18 Dec 2015, and I visit my oncologist later
today, 7 January 2016. ADT hormone
therapy continues with Psa is not going down as far or as fast as
it has during past applications of Eligard and
Lucrin.
The graph gives my Psa history which explains how my treatment for
prostate cancer has proceeded with
ADT and Radiation. My conclusion at present is that Psa is not
being held down to the initial levels achieved
when ADT began in April 2010. Since then, I've had two pauses from
ADT, and during both the Psa rapidly
rose indicating that radiation did not have much effect on cancer
cells. The underlying value of Psa from 2011
to present 2016 shows that it is slowly rising, and testosterone
is not being fully suppressed by Lucrin injections.
I can see that if the slow rate of increase of my Psa continues,
it probably will indicate Pca is going to spread
and kill. Its what cancer does. Use of alternative therapy such as
apricot kernels, about 24mg per day of amygdalin
seemed to have zero effect on Psa over a long time of intake.
Cannabis oil with low THC, high CBD seems to
have done nothing between Feb 2015 and October 2015. My daily dose
began at 0.2mg, a very tiny amount,
but it was enough to get a strong high. Sensitivity slowly reduced
and at end of period I could take 5mg.
I stopped taking it Oct 2015, and experienced no withdrawal
effects. It has been totally non addictive, and
gave me good inner calm feeling about life.
Websites promoting cannabis for cancer cures should be considered
snake oil treatments until proven otherwise.
There have been NO studies of social groups of ppl who regularly
smoke or ingest cannabis products, such as
those living in Jamaica et all. I might guess that any studies
might show there are no reductions in cancer rates
where it is widely consumed and in tropical regions where it grows
so easily it is hard for authorities to eliminate.
I might add that prostate cancer rates are worst for those with
dark african genes, and there is considerable
variation in rates for different races or genetic blocks of men.
There is no way yet for a man to alter his genetic make up to not
endure prostate cancer. Some websites
promoting cannabis oil say you need to take a GRAM a day but this
seems utterly wrong. One gram = 1,000 mg,
and has volume = 800 cubic millimetres. I doubt I ever took more
than 6 cubic millimetres a day, a small drop
on the end of a little metal spatula I made. So, assuming I
averaged 5 mg a day for 270 days in 9 months,
the maximum I would have used was is 1,350 mg, or just over
1.35grams, or less than 2 cubic centimetres, 2cc,
and not much from initial supply of about 20cc, or 16 grams, which
was obtained by my friend from about 300
grams of harvested Sativa heads.
The oil yield rate is extremely low compared to rate for the
Indica variety that has been subject to genetic
selection since 1970s when Indica began to be grown commercially
by hard nosed arsolic criminals who want
the product to give a huge high for a small amount which is
cheaper to grow. The Indica sold in most underground
sales is "skunk" and very high in THC which has psychotic large
effects so beloved by those subject to becoming
hooked to drugs. There is a very low % of CBD oils in skunk, and
its these oils which give the calming effect, and
boost to immune system, if there is any to be had. It turns out
that our bodies produce CBD chemicals naturally for
immune system and calming function. Therefore skunk sold on the
streets is having a very bad effect on the hoards
of stupid young people who foolishly believe they can ease the
pain of their existence by getting high, and the then
so many suffer schizophrenia or other disorders which make then
useless for anything, unemployable, and
dependent on welfare. I should know, because I have a nephew who
succumbed to mental illness while trying to
keep up with his 2 older brothers, one of whom sold pot to
classmates at age 12, and who went on to become a
bankrupt at 23, after dabbling with heroine given to him by a girl
friend. The other brother dabbled in cocaine.
These three young ppl had Shit For Brains in the formative years;
nothing could be done to get them on the straight
and narrow. They were always allergic to hard work.
So I really do know about cannabis and its effects. My friend who
prepared my oil for me did not dilute the oil at all,
and in fact it was a dark brown grease, unable to flow.
Had I had tried to take 1 gram of the oil I had daily, I would
probably have become extremely ill. It may have had
such a huge psychic effect that I could have a fall or other
accident in the house and done myself an injury. It may have
been fatal. Websites promoting cannabis oil for health say the
high from THC need not be strong, just be present,
and still allow you to live independently without risk of
accidents, despite the feeling of "being remote" while cooking,
or watching TV. The guys promoting "Medical Cannabis" will insist
on telling ppl they need 1 gram a day. The density
of oil = 0.8 grams per cubic centimeter.Therefore 1 gram of oil =
1 / 0.8 = 1.25cubic centimeters = 1,250 cubic millimeters
= 1,250ml.
The guys selling oil know that ppl only need 2.5ml per day of oil
to get a high especially with skunk or a new user taking
it for medical reasons. I have seen websites saying you need 60
grams or 1 gram a day for 2 months for a cancer cure.
The active ingredient of raw oil might be 60 x 2.5ml = 150ml =
0.15cc. To this they add 75cc of canola or olive oil,
so the bottle contains 75.15cc of diluted oil.
They have diluted the product by a factor of 1/500. The price is
only $10,000 - to save your life. The price they get for
the raw THD ingredient in medical cannabis paid by gullible
non-street wize ppl is far better than the price ppl pay for
the same amount of THC to ppl who need to smoke 2 bongs a day.
There is no evidence cannabis oil cures cancer.
With the oil my friend provided, I certainly got a high always
with less than 5mg. It seemed so "strong" at times that it i
s strictly a stay-at-home substance, you MUST NOT tempt fate by
driving a car, or doing anything in a workshop.
So this "therapy" is a "mind zonker", even with this variety of
Sativa which is just a natural wild variety which has not
been genetically selected to make the THC much higher and CBD
lower. The Sativa oil had me "good for nothing a
hour after taking it." I found I never ever had feelings of
paranoia which are the hallmarks of psychologically damaging
varieties of Indica cannabis which are very high in THC and with
hardly any CBD should be avoided at all costs,
especially by teenagers who can succumb to schizophrenia and other
mental illnesses. Natural Sativa variety is low
yield, low THC. And anyone 16 who reads this will not have the
slightest idea about what he is buying, and what I
say here is all bullshit.
There are ppl very prone to addiction to many things; 80% of
alcohol is purchased by 15% of the population,
80% of gambling is by 10% of population who are problem gamblers.
Studies would show 80% of recreational
use of drugs is by 15% of population, with a good number becoming
addicted. Tobacco was once smoked by
50% of everyone I knew, with probably 25% smoking twice as much as
the other 25%. I once smoked up to 15
cigarettes a day, then said I'd give up, cold turkey, at age 34,
when a GF at that time said I stunk like a chimney.
I did give up, cold turkey, but GF went through usual cycle of
Love, fading to co-existance, then Hate, and off
she went to roam and slut around
world - again - like the year before, in between the years of
being employed as a primary school teacher where
she could not last longer than a year without getting fed up, and
needing to piss off. This was typical of the many
useless dreadful young women I met who could not settle down with
anyone. Their efforts to relate to me were
120% un-respectable. Sex wasn't especially wonderful, just sex. I
don't have an addictive personality, and cannot
be addicted to fraudulent lovers, grog, cannabis or anything else
at all. The cannabis oil had me sleeping better,
calmer, less worried, less anxious, and being more able to accept
my dismal future. I didn't like being forced off
the bicycle with knee pains. There is nothing nice about declining
with age and slowly losing every ability all
ppl under 50 take for granted. Aging means everything known and
practiced as "human life" becomes very
limited, and denied to ppl when they get older.
-----------------------------------------------------------------------------------------------------------------
12 October 2015.
HT was restarted 1 August 2015 following Psa 3.3 level 10 July.
Psa is going down again.
13 July 2015. Since February 2015 little has changed with my
health, except that my knees are beginning
to wear out and I cannot ride a bicycle as fast. But I have
finally given up any desire to go fast as I could all
the time. My Psa has risen from about 0.4 in Feb to 3.3 at 10th
July 2015, so you can see that there is a very
fast doubling time. An acceptable doubling time is say 10 years,
so from 50 it goes from 1.0 to 2.0 at 60, then
4.0 at 70, and 8.0 at 80, and maybe you last until 90.
I have a cousin of 70 who has Psa = 0.3. There is a good chance he
had a lower testosterone level than I did.
In my case, I have paused from hormone therapy after February and
its effect has down over 3 months and
my body has resumed testosterone production. Prostate glands
normally generate a high Psa marker chemical
in blood due to testosterone presence, and it does this even when
no cancer is present. Normal range
of Psa on pathology results is cited to be from 0.3 to 5.5ug/mL
but this is misleading because what is
normal when you have been previously diagnosed with Pca?
I've known men whose Psa was 18 but there was no Pca. Well, not
yet.
So "Normal" is a silly word, and 0.7 at 40 and 1.0 at 60 should be
the standard.
THE DOUBLING TIME of the Psa level is much more important that the
actual level if the level is "normal."
I had no surgery. I was radiated, so the prostate gland is just
sitting there like an internal crouching demon
ready to mutate and grow uncontrollably. So whatever Psa chemical
is produced, it could be from cancer
cells, or from normal cells. But not one doctor knows the exact
state of my prostate gland or if there is any
metastasis. They are only guided by Psa level and its change and
the statistics.
Having low testosterone < 0.5 ( normal range 8 to 38units ) in
most males will reduce Psa to less than 0.5.
The pause in HT is supposed to do my body good to allow some
return to having testosterone and to see if
the EBRT in 2010 has worked over time.
This is the second pause in HT I've had, and this time the mental
change has been negligible. My bike speed
has reduced and general daily desire for sex and ability to "fix
the itch" has not returned. Well, maybe it is
mental, because at 68, there is not a woman alive who'd ever want
to be with me in any way. I have moved
to the age where I am naturally repulsive to 99% of sheilas. Most
are far too polite to mention this fact, because
politeness is something many of them discover is the key to a
peaceful sexless life without arguments with men,
usually over money, and getting their own way.
It is maybe 20 years since anyone actually touched me with care,
except for medical professionals paid over
$100,000 pa. Its OK, I just handle it, rather like my mum of 98,
who hasn't had a man touch her since she was 55.
I have become polite enough to enjoy women's company without ever
having them feel frightened, angry, or
sexually aroused when it is not wanted.
The Psa rise during 2015 is just like what occurred in early 2012,
indicating cancer tumour is alive and well, and
intent on killing me. See the graph above for Psa after January
2008.
Psa rode from 4.3 to 6.3. I was diagnosed after biopsy in late Dec
2009 with Gleason 9, aggressive cell type,
young man's type of cancer, prostate gland was 3 times normal
volume. Biopsy gave 9 live samples of 9 taken
through rectum wall, a very painful experience with no
anaesthetic. Open surgery was attempted April 2010,
but abandoned after cutting me open. Cancer had just advanced
beyond capsule but had not spread.
ADT with Casudex followed by Eligard was commenced, and In Dec
2010 I had 35 RT sessions when Pg had
been shrunk to smaller size due to ADT. Eligard was injected once
every 3 months causing temporary chemical
castration. I am presently (12 October 2015 ) back under effects
of re-started ADT
with Lucrin injections. Psa has fallen, but probably I will never
lower it to the 0.08 back in April 2012.
The effect of ceasing and re-starting ADT shows Psa rise and fall
similar to between 2012 to 2013.
The latest peaking rise in Psa indicates it is likely the
radiation treatment has done little if anything to prevent
prostate cancer from finally killing me even if I remain on HT for
however many years Unkel Nature has
allotted to me. The graph shows an underlying rise in Psa at
nadirs during ADT, and doubling time from August
2013 to April 2015 = 16 months. From this I could say that Psa in
6.6 years time might be 32, aged about 75,
and I may not be very well. The idea of living to my 90s would
depend on a miracle cure.
There are some miracle cures one hears about, most one hears or
reads cannot be taken seriously.
There's a drug called Keytruda which works for melanoma well, its
now available on PBS scheme in Oz.
It is said to work on other cancer types including Pca, but then
it is new, and trial results are yet to be finished,
so I doubt my oncologist is going to prescribe it for me in 5
weeks when he gets back from his winter holiday.
So knowing what the latest cure or treatment may be is fine, but
so often we hear BS about something that won't
help us in time.
-------------------------------------------------------------------------------------------------------------
Last July 10 2015, 3.3.Previous Psa June 2 2015, 1.4.
The 2015 Psa rise is similar to rise in 2012 when I paused for 6
months from HT injections.
I will start again with HT next week with Casodex tablets followed
by Lucrin injections to reduce testosterone
to low levels.
I have no cause for optimism, and alternative remedies such as
apricot kernels and daily cannabis oil for last
5 months have done absolutely nothing to change the shape of the
curve for Psa rise. Had my Psa risen to only
1.5 with a then begun to fall, the HT + RT could have been said to
work, but as I see it, its only a matter of time
and I would bet that when I re-start HT the Psa will not drop drop
to levels on early 2014, 0.26.
--------------------------------------------------------------------------------------------------------------
6 February, 2015.After an aborted attempt to remove my PG
surgically in 2010, I was given HT for 2 years
with a full course of 35 RT in Dec 2010. After 2 years of ADT Psa
went to a low 0.08. I stopped ADT, but by
May 2013 Psa climbed to 8.0 and free Psa indicated Pca was
progressing. I started a second round of HT in
early June 2013. By the time the effects of the last injection of
Lucrin ceased by about April 2015, I will have
had ADT for 22 months.
The Psa nadir during the second round of ADT has been 0.2 in April
2014. Psa has risen slightly to 0.36
last month, indicating a doubling time of 1 year. This does not
mean the HT has become ineffective.
The PG cells I have are radiation affected and some may be
healthy, and these produce a Psa reading along
with any cancer cells, and it is difficult to determine where the
source of Psa really is, because the HT reduces
Psa produced by both healthy and cancer cells - while the HT
it remains effective.
During my last visit to my oncologist at CH, he and I decided to
quit the ADT and watch the total Psa to see if
it rises rapidly and determine free Psa which will indicate if the
cancer is progressing. The oncologist says a pause
in HT to allow a return of testosterone production will be good
for me. If total Psa remains below 1.0 then it may
be considered the Pca is in remission but that if it rises above
1.0 - and rapidly - then I will have to return to HT.
I will not have a Lucrin injection at end of this month when the
next injection was due. I might assume my
testosterone will begin to rise in about April, and I will have a
Psa test in late May, just before I see my
oncologist in early June.
I may need to remain chemically castrated for the rest of my life.
Castration affects men in a variety of ways, and there are many
myths. There is no feminizing apart from some
body hair reduction. Drugs like Lucrin or Eligard which suppress
testosterone production do not cause feminizing
effect like female estrogen, sometimes given as ADT. So I shall
not grow breasts any time soon, or hear rise in pitch
of voice etc. I doubt I suffer depression, and I can keep my
weight under control, now 83Kg, with BMI = 24.8.
But of course I am ageing, and although I am same weight as I was
when at my fittest when 41, some muscle has
been replaced by fat and there's nothing I can do to stop this
while on HT and and under effects of zelodronic acid
to prevent bone thinning.
Unfortunately, many men find themselves depressed by ageing, and
so many cannot ever control eating, drinking,
laziness, and social habits which are all bad. I'm the exception.
Many men blame weight gain and the and drift to
other illnesses on medication, and by 60 they become ugly
caricatures of what they once were, and they give up
on themselves. Their wives also to the same thing, and its no
wonder depression is so common, and desire for
vibrant intimacy has become a thing of the past.
It's been 37 years since I was married, and I'm still looking for
a partner and I definitely can function sexually.
So while single, I have nobody to displease by getting old and
getting a few health problems. I find most ppl
avoid relationships like the plague after age 45, but I'd welcome
one. The difficulty is in "chemistry", and most
women have zero desire for a man after their menopause, ie, they
have "paused from men", and no amount of
chemistry, charisma, or money, care or anything else will make any
relationship possible. There are thousands
of females over 30 advertising on dating sites wanting men. Let us
suppose 50% are bogus creations by website
"managers", ie, arsole scamsters. The remaining 50% run a mile if
a man does suggest a meeting; they say they
want a man, but most are quite incapable of following through with
active pursuit accompanied by watchful eye
to sort out who is or is not a member of the army of men from
Arsolia or Bastardia where all manner of fellows
really want to be euthanized tomorrow.
I continue to cycle a constant average of at least 200km per week
to keep fit. Very few fellows overtake me
during my rides. There seem to be virtually no men my age still
cycling. I rarely EVER see any woman over
40 on a bike, and 95% of all the females on bikes don't want
anything to do with me; I am an old fart, and they
cannot keep up to my speed, despite them being perhaps 40 years
younger, and me having bad knees and lack
of speed due to muscle weakness aided by chemical castration.
I probably have high willpower levels, so after July 2014 I gave
up wine and chocolate and last Xmas gave
up having a cookie during each cafe stop while out on the bike.
The ONLY way a man or woman can prevent
fatness by eating less calories than consumed by exercize, ALL THE
TIME, until they die. Between 1993
and 2006 I stopped cycling and doing building work due to knee
pain - I have bad knees. So during 13 years
I put on 19Kg, which works out to 2.7 grams per day. This seems
like such a tiny weight gain, and ppl hate to
think something so small matters so much, but while living a
sedentary life you just have to reduce calories far
more than one might think is sensible.
I have GFE genes - Get Fat Easy. The only way for me to control
weight is to weigh myself EVERY morning
using electronic scales able to resolve to nearest 0.1Kg at least.
Then I plot the graph of weight in my daily
diary, and if any jump in weight occurs, I fast, and ride a a bit.
Over 2 months you will see variations in weight
of +/- 0.1Kg, but you can SEE the TREND of your weight, and read
the average weight for each month.
I allow a Supreme Salad Sandwich every day at my favorite
restaurant, the "Siam Twist" at Hackett in
Canberra.
Do not believe the poor reviews about the Siam Twist; it is
luxuriously pleasant.
http://www.tripadvisor.com.au/Restaurant_Review-g255057-d7110784-Reviews-Siam
_Twist-Canberra_Greater_Canberra_Australian_Capital_Territory.html
With two large cappuccinos, its under $16, which I can afford.
Once a week I have a Thai dish, Duck Salad
or a Laksa with noodles and tofu in winter. I enjoy occasional
male company and newspapers to read, very
pleasant staff, and so I enjoy being away from home.
My knee osteo arthritis is beginning to limit what I do on my
bicycle, so as long as I don't ride more than
300km within a week I am OK. I am not yet begging an orthopaedic
surgeon to install titanium knee prosthesis
to both knees. It may happen, but I'd have to wait a year before
getting the operation and my cancer progress
may prevent the operation if the docs think I will die sooner
rather than later. Right now, the oncologist does not
think my prostate cancer is spreading. I don't need to ever walk
further than 200M ( carpark to movie theatre ).
I doubt I'll ever need to walk further, say, along a beach at
sunset with a beloved. If I try walking on sand my
ankle injury from a motorcycle prang at age 19 has me completely
disabled.
Women dream of romance and expensive resorts, but they need to be
able to be happy right here and right now,
and then all days following the day you meet them. They should
never need to travel anywhere, but I make an
exception for coming out with me on a ride. Like many with leg
injuries from a past life, I can cycle OK.
A bicycle is just a wheel chair with one wheel in front of the
other.
For last few months I ate an average of 40 apricot kernels a day
as alternative therapy which is claimed to
stop cancer spread. I doubt its having the slightest effect but
then it seems a benign dietary supplement,
although they do cause some bowel irritation. I have have a friend
with a HERB which I will begin to take
soon; I cannot say more about it, but if it appears to lower Psa
after going off ADT, I'll let you all know a
bout it.
I now know of 3 local men who had what seemed to be successful
surgery giving extremely low Psa.
All have complete ED, and most have enough continence. After a few
years of having Psa < 0.02,
Psa rose, so one had additional surgery to remove his bladder and
have an external bag fitted, another had
all the RT that I had, and another has Psa of 0.05 after 4 years
and he probably will try HT and or RT, and he
much fears the Psa rise at age 75. So even if the cancer is
removed surgically, some small amount of prostate
gland cells may be left behind, and they too may eventually become
cancerous, if they were not already at
time of surgery.
In my case surgery was not possible despite a fairly low Psa at
diagnosis in 2009. I still have a prostate gland
which is probably much affected by RT, but exact status of
cancer cells is quite unknowable. Therefore it seems
pointless to worry too much about a Psa which is 10 times the
level which alarms other men so much after they
have had surgery. I expect my Pca to kill me; the doctors said
they just don't have a cure.
Life expectancy for a man in Oz is now 84 years, but that just
means very many die well before they turn 84.....
Sure, a few live to 104, but I don't expect to one of them.
----------------------------------------------------------------------------------------------
For anything before 6 February 2015 :- Past history.
My variable interest in road cycling :- Velosophy
To
Index Page